This blog covers skin scars only but does not include burn scars or scars related to breast implants.
Virtually everyone who lives long enough will have a skin scar from elective surgery or an injury. There has been a barrage of cosmetic surgery procedure modifications to decrease total incision length in the hope of creating less scarring. The healing of these disruptions in the skin surface follows a specific process. After the injury or cut there is bleeding. Once this stops an inflammatory process starts to get the cells needed for healing into the wound. New blood vessels grow into the area bringing in the energy needed to complete the healing process. You see this as a red color of the scar and the skin immediately next to the scar that blanches white with finger pressure. Within a week or two the healing is sufficiently strong that the wound should not reopen and any sutures that were placed can be removed. Even though the wound is healed it then must mature over the next 6 to 9 months depending on the type of injury, affected body part, age of individual etc. before the redness goes away and the increased blood flow is no longer needed. Once the scar has fully matured it usually does not blanch with finger pressure. Any problems in this process such as an infection, failure to suture a wound closed, certain vitamin deficiencies etc. prolong the healing time and in doing so result in worse more visible scarring. The skin of younger individuals makes strong repairs and tends to over heal, resulting in larger, thicker scars than on older skin. Skin over the jawbone is tighter than skin on the cheek and will tend to increase a scar’s prominence. All scars are more amenable to treatment early in their life span before they mature. It is easier to prevent a bad scar from forming by control/manipulation in the early phases of wound healing than to treat one that has already formed.
Typically, a scar will become increasingly prominent at first. The tissue increases in height, firmness, and redness (vascularity) and then gradually fades. Many disfiguring marks which seem unsightly at three months may heal quite satisfactorily if given more time. The desired end result is a flat (not indented or raised), soft, pale, less than 1mm wide scar. We can call that the normal scar. The non-normal scar is more visible due to a number of factors, including its difference in topography (surface contour or depth and height relative to adjacent skin), color, thickness, pliability or texture versus the surrounding normal skin. Scar length, width or direction can also contribute to visibility. A scar that crosses natural expression lines (Langer’s lines) or wrinkles will be visually striking because it will not follow a natural pattern for example a scar that obliquely crosses the natural skin fold between the corners of the mouth and the nose is much more visible than one that lies along this fold. If the skin scar adheres to deeper structures such as muscle or bone the skin may bunch up with movement as it is tethered to deeper structures and that also contributes to visibility. In fact some scars may only become visible on animation or movement. Some scars are accompanied by a loss of skin with or without a corresponding loss of deeper tissues (a tissue deficit). In worse cases the patients complain of scar itching, pain, breakdown to a raw surface with minor trauma (an unstable scar) and even recurrent infections in addition to scar visibility. I take all of these factors into account before treating a patient with scars and then develop a treatment plan specific to the patient’s situation.
White scars are visible because they have lost all of their pigmentation. Excimer laser or dermal needling (a tattoo like needling of the skin without tattoo pigment) can be used to stimulate pigment cells to migrate into these types of scars from adjacent non-scarred skin. A more expensive approach would abrading the surface of the scar and spraying pigment cells harvested from elsewhere on the body onto the surface of the wound. The cheapest approach in such cases is camouflage make up.
TYPES OF SCARS
The non-normal or non-desireable scars can be classified as significant skin loss/deficit, flat and wide, hypertrophic and keloid.
–SKIN DEFICIT
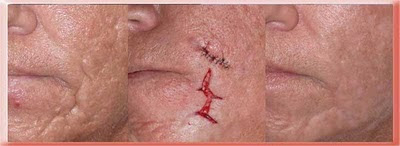
These scars usually arise after injuries like bites and car accidents where the skin is disrupted by an object that is not knife sharp. The skin at the edges of the wound is crushed in the process and either dies on its own or has to be cut away by the surgeon.
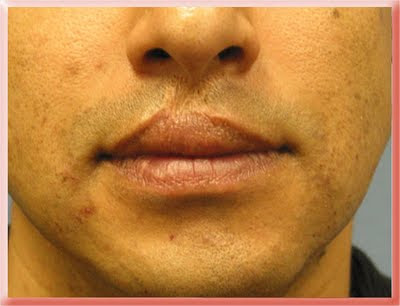
This patient had a scar with significant loss of skin that shortened the vertical length of the central upper lip and distorted the normal lip proportions.
–FLAT AND WIDE
The final scar width is dependent on the tension of closure and distracting or separating forces applied to the scar with movement before the scar has fully matured. If an injury causes a wound and crushes skin at the edges of the wound that crushed skin is usually removed. The non-crushed skin at the edges is of better quality but when the edges are sutured together it may be under tension from skin loss and that leads to a wider more visible scar. Alternatively the scar may lie along the scalp, front of the knee or back of the elbow where movement will constantly stretch the scar along the length of the limb or skull before it has fully matured and widen it. The visible linear scar of the scalp can be a cosmetically serious complication of a scalp incision in scalp surgery, forehead lift or craniofacial surgery, especially on the temple scalp where it is harder to hide by combing the hair over it. This area of hair loss is usually due to incisions or cuts that damage the hair follicles along the cut or laceration as well as widening of the scar line after healing. Treatment limited to removal of skin only increases tension around the scar and results in a high recurrence rate of these types of scars.
I had a patient with a scar over the jaw line that would alternatively turn red and then
pale as the patient moved his jaw -speaking, eating, or making facial expressions. This was due to the tension applied across the scar with jaw motion.
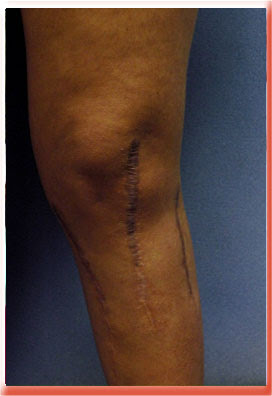
This photo shows a knee scar after orthopedic surgery. The scar is wide and flat and lies over those parts of the knee that are constantly placed under tension with knee movement. You can test this for your self by pinching the skin over the while the knee is extended. When you then flex the knee you can feel the tension of the pinched skin that would be applied to a scar over the knee with knee motion. Also note the small punctate scars along side the main scar these are stitch mark scars from the sutures. The scar is widest where it lies over the joint itself due to the greater amounts of tension across the scar. The scar is normal over its lower third because of the absence of tension across the scar. These scars are best treated by taping the scar for some months after surgery. Once they widen it is very hard to fix them because of the motion at the joint and the increase in tension when you remove any skin as you would be doing if you cut out the scar.
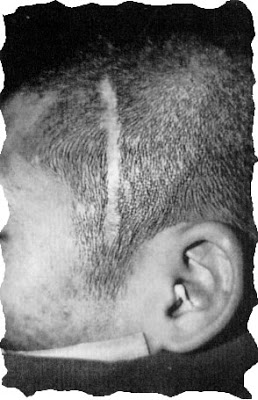
This is the type of scar seen after injury or cosmetic surgery (browlift, facelift). It is much harder to hide one of these types of bald scars on the side of the head than on top of the head where hair can be combed over it. Although the scar may be of good quality the associated loss of hair along the scar makes it much more noticeable than it otherwise would be.
–HYPERTROPHIC
Hypertrophic scars are seen as a ridge within the confines of the original wound. They develop soon after surgery, usually subside with time (mature), are confined in size/growth and usually occur across moving areas of skin (abdomen, palm, front of the elbow, in the fold under the breasts). They are thickened scars over areas of skin compression. They can also arise from a prolongation of the healing process. More tissue than is required is produced to close/cover the wound. They can be a single raised line along the scar (linear) or a raised area of variable shape (widespread).
–KELOID
Keloids appear sometime after the original surgery or injury, rarely subside with time, grow out of the confines of the original wound, (a minor injury can produce a large keloid), are independent of skin motion (such as earlobe keloids), rarely occur across joints and can become much worse after surgery without concomitant steps to prevent recurrence. The incidence of keloid scarring increases in darker skinned individuals but not ever darker skinned individual gets them. Despite that my keloid patients are mostly Afro-American followed by Asians and then those of non-European Hispanic descent. I have only had a few Caucasian patients with this problem. Keloids have not been reported in albino’s of any race, suggesting a potential role of skin pigment in this type of scarring. There is an increased incidence of keloid formation running in families so it is inherited to some degree. Keloid scarring does not follow the same pattern of evolution, stabilization, and involution of the normal or hypertrophic scar. It may develop directly after an initiating event or some years later, arising from a mature scar. Earlobe keloids usually occur months are years after the initial ear piercing. Keloids also can occur spontaneously. Virtually all keloids that are cut out will return if steroids and pressure are not applied after surgery. In some cases radiation may be used instead of pressure.
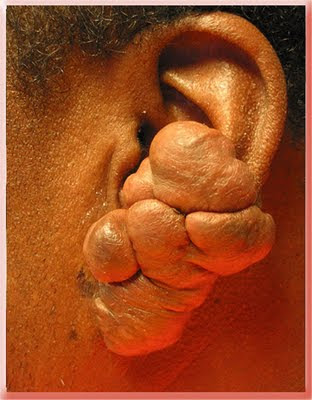
This patient had a keloid from an ear piercing removed with inadequate care afterwards to prevent it from coming back. It of course grew back and you can see how it grew out of the boundaries of the original piercing so that it began to block the ear opening and affect hearing.
A scar can have mixed properties along it’s course for example a midline scar extending down from the chest into the abdomen can be normal in the upper half and hypertrophic in the lower half or the mixed scar in the knee photo above.
TREATMENT
The goal of treatment is to make scars less visible and relieve itching and pain if present. Silicone gel sheeting and corticosteroid injections into scars are the only treatments for which there is sufficient published medical journal evidence to justify their use. Studies of scar treatment are complicated by the natural tendency for scars to improve over time. Having said that most physicians including myself rely mostly on what has worked for our patients rather than referring to published studies involving large groups of patients. Looking at the accompanying photos you can judge for yourself what is effective.
Frequently a combination of treatment modalities is required because not every modality works on every patient or scar by itself. When applied together some modalities have a much greater effect than the sum of their individual contributions.
–SURGERY
Surgery is commonly used to cut out a scar. The resulting sutured wound creates a young immature scar that responds better to the modalities described below. In the case of tissue loss new skin can be brought to the area by skin grafting or small surgical procedures to move around adjacent skin. Surgery can also be used to break up a scar, detach the scar from deeper tissues, change scar direction or manipulate adjacent tissue to decrease tension along the scar line -all of which can make a scar less visible. These procedures are usually performed under local anesthesia so the patient does not have to go to sleep under general anesthesia. Surgical removal alone for keloids without any of the adjunctive procedures below has a 45 to 100% recurrence rate. This treatment modality is the one I most commonly use on my patients.
–SILICONE GEL SHEETING
Silicone gel sheeting has been in use since the early 1980s for the treatment of scars and has been proven to be effective. It is available over the counter as a solid sheet or a gel that you apply which hardens. Despite its track record my patients have not liked it and it has not been effective in my practice.
–PRESSURE THERAPY
Pressure has been used in the treatment of scars since the 1970s. The effectiveness is dependent on how long the pressure is applied for. Some doctors recommend 6 to 9 months of pressure but the majority of my ear lobe keloid patients only require 2 to 3 months of pressure earring wear. Certainly scars that have recurred after previous treatment should have pressure applied for a longer period of time. Scar massage has the same effect as pressure with the additional effect of breaking up scar connections between layers of tissue.
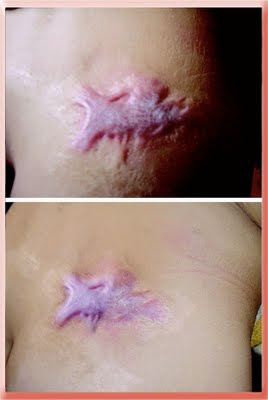
This is a widespread hypertrophic scar on the right buttock. After 6 months of pressure applied to the scar the part of the scar that received pressure is flatter. Pressure definitely works if applied long enough.
–CORTICOSTEROID INJECTION
Corticosteroids are most effective when injected and not so effective when applied topically (except when applied as a medicated tape). This is the second most common modality I use on my patients, mostly in conjunction with surgery and it has been in use since the 1950s. Only very small amounts of the appropriate strength should be injected at a time very close to the surface in order to avoid thinning or depigmentation of the skin or creation of spider vessels around the injection site. If too much is injected too deep into the skin the risk of these problems occurring goes up. Except in the case of keloids the injections should not be closer than 4 to 6 weeks apart in order to avoid these problems as well. When used together with surgery for keloids the recurrence rate drops below 50% .
–RADIATION
Radiation applied right after surgery for keloids drops the recurrence rate down to 10%. 4 treatment sessions are required. Despite that I have found that the majority of these patients will require corticosteroid injections and/or medicated tape to get the best result. Although the keloids do not come back these scars tend to hypertrophy but are very sensitive to corticosteroid treatment.
–LASER
When the ablative lasers (those that vaporize surface skin) appeared in the mid-1990s the general public was lulled into believing they caused less scarring than scalpels. This turned out to be science fiction. There is no advantage to using these types of lasers in surgery to prevent scarring or to treat scars. The lasers that obliterate small blood vessels near the skin surface without destroying the skin have shown some promise in treating and preventing the formation of bad scars but multiple treatments are required and the best results are those given in combination with other treatment modalities like corticosteroid injections.
Some doctors have reported using fractional lasers, which make very small separated holes in the skin surface, on hypertrophic scars and achieving satisfactory results. Others use the fractional laser on keloids to soften them and report a greater effect of injected medications into the keloid afterward.
–DERMABRASION
Dermabrasion involves the application of a rough surfaced rotating device to abrade the surface of the skin. It flattens scars the way sanding a wooden surface makes it smoother. Dermabrasion in general is much less commonly performed than it was prior to the introduction of skin lasers.
–FREEZING – CRYOTHERAPY
Freezing scars has been used in the past but is not currently popular because of the high risk of damaging pigment and the creation of scabs that take some time to heal over and separate, especially if the freezing agent is applied externally. In 1993 doctors began injecting the freezing agent into the keloid. In 2002 a new device was developed, CryoShape, to make injection of the freezing agent into the keloid easier.
–TAPE
This is the modality I use the most after surgery both for scars and after cosmetic surgery. By applying the tape you decrease motion along the scar line and it is preventative against wide flat scars. The greatest advantage is that it is cheap and easy to do. It is not effective for the treatment or prevention of keloids.
–CORTICOSTEROID MEDICATED TAPE
Over the years I use more and more medicated tape in my patients. Patients that respond to corticosteroid injections but require more than 1 or 2 injections get this treatment. The medication is mixed with the adhesive and the tape prevents the medication from evaporating so it can be absorbed into the skin. This treatment has been a lifesaver for many of my patients, and me also.
–CAMOUFLAGE TATTOO
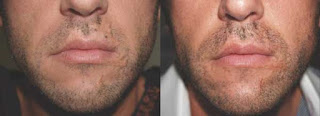
This is reserved for men who have scars on the face with loss of the beard hair in the scar. The medical tattooist tattoos small black dots to match the facial hair and the result can be very good. The only problem is the tattoo may fade over time and require touch ups.
–OTHER MEDICATIONS
Interferon an immune medication and some cancer chemotherapy medications have shown effectiveness in scar treatment when injected in small amounts into the scar. Currently these are not the most popular treatment modalities.
–SUNSCREEN
Sunscreen should be consistently used to protect scars from sun exposure until they have fully matured in order to prevent the scars from becoming permanently hyperpigmented (darker).
The company Crescendo marketed of a drug called, HybriSil (methylprednisolone acetate 1% in silicone gel), for the treatment of skin scars. The idea was that combining a topical steroid with silicone to the skin surface was beneficial. The problem was this combination had never been placed through FDA required trials. In November 2011 the FDA sent them a warning letter that Hybrisil was illegal because it had never been approved and was being misbranded. It was an unapproved new drug product, which could not be marketed without approval by the FDA based on data showing that the product is safe and effective for its intended use. It took Crescendo until January 2012 to file an investigational new drug (IND) application that permitted the limited distribution of the product for investigational use only.. The FDA made a return inspection of Crescendo in late January 2012 and determined the company still was distributing the product for noninvestigational purposes and the labeling failed to carry adequate directions for use.. In early May 2012, the FDA ordered Crescendo to discontinue manufacturing, and the company agreed. The FDA said it has not received any reports of adverse reactions associated with HybriSil. The company reports that it has begun clinical trials and intends to work with the FDA to secure approval of a prescription HybriSil, and eventually, an over-the-counter version but that does not change the fact that it tried to circumvent the drug approval process.
CASES
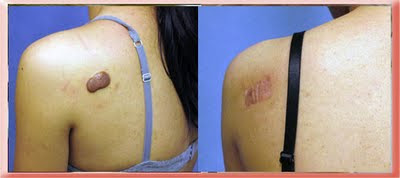
This patient had a keloid arising in an acne scar. I could not cut it out because there was not enough surrounding loose skin so I shelled out the keloid at surgery. Radiation and medicated tape were used after surgery and the after photo is 7 months after surgery.
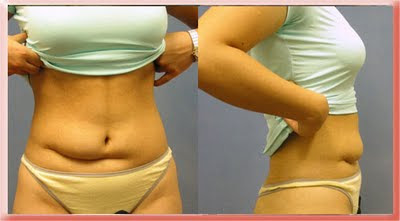
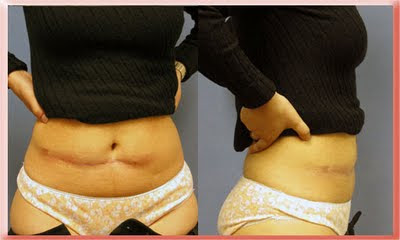
In this case the scar from previous surgery connected the skin to the stomach muscles. The surgery involved separating the deep from the superficial layers and a little bit of liposuction to even the surface contour. The after photo was taken 1 year after surgery.
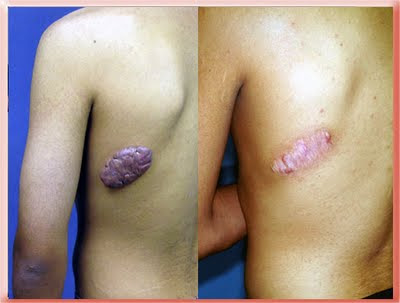
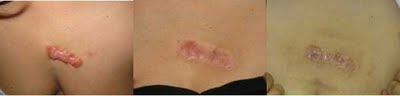
This patient had a keloid on his back that was removed elsewhere twice and grew back within 2 months of surgery. There was enough loose tissue around the keloid that I could cut the whole thing out. Radiation was used after surgery and then taping. This patient did not wear the tape as directed and so the end result was a wide flat scar but that was still better than a keloid. The after photo was taken 1 year after I did this surgery.
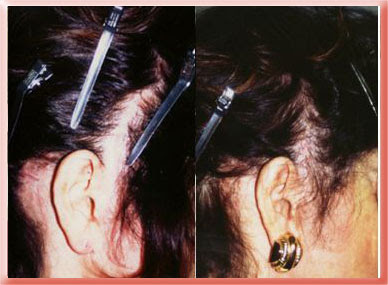
This patient began losing hair 1 year after a facelift by a surgeon other than myself. She had a wide flat bald scar on the temple scalp and hair loss behind the ear. I grafted hair from the back of her head to hide these scars.
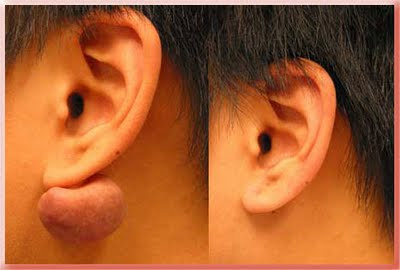
For this patient I surgically removed the keloid under local anesthesia and then treated with corticosteroid injections and 2 months of pressure earring wear.
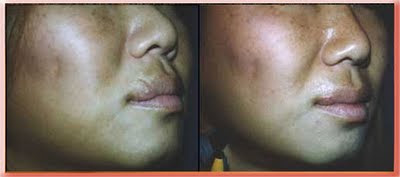
In this case I removed a wedge of scar tissue and damaged lip and then realigned the lip margins. The only treatment modality required was surgery under local anesthesia.
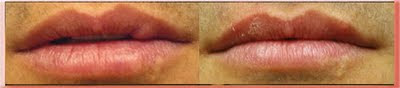
This is one of the easiest scars to treat. I removed the hypertrophic scar under local anesthesia and just sutured it. No additional treatment was required. The hypertrophic scar appeared because the original wound was not sutured.
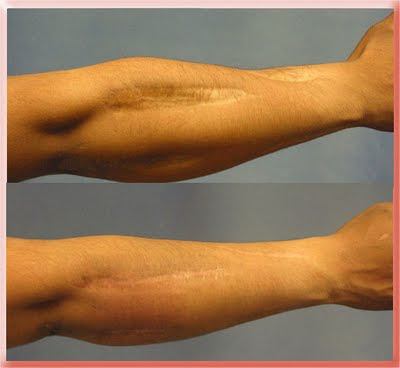
This patient was left with wide depressed scars on his arm after limb saving surgery in another country. The skin could not be sutured at the time and that contributed to the scars. I stretched the adjacent skin with sutures for a month or two before cutting the scars out. That allowed me to close the excision sites with less tension and decrease the chance that the scars would widen again. The after photos were taken about a year after surgery.
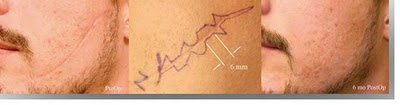 This scar is visible because it lies in the middle of an aesthetic unit of the face and is not aligned with any naturally occurring facial skin folds or wrinkles. The treatment is to excise the scar with irregular geometric shapes to make it less noticeable. If you used only one shape such as a triangle the result would not be as good. Photo courtesy of Dr. David Hendrick
This scar is visible because it lies in the middle of an aesthetic unit of the face and is not aligned with any naturally occurring facial skin folds or wrinkles. The treatment is to excise the scar with irregular geometric shapes to make it less noticeable. If you used only one shape such as a triangle the result would not be as good. Photo courtesy of Dr. David Hendrick
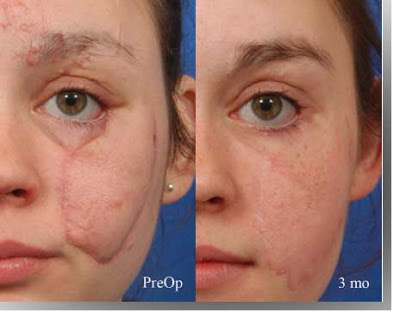 In this case a circular scar causes the skin within the confines of the scar to protrude outward. The treatment is to make the scar zig-zag and thin the fat layer within the confines of the scar. Photo courtesy of Dr. David Hendrick
In this case a circular scar causes the skin within the confines of the scar to protrude outward. The treatment is to make the scar zig-zag and thin the fat layer within the confines of the scar. Photo courtesy of Dr. David Hendrick
In some cases it is best to just cut out the skin scar and suture the resulting wound closed.
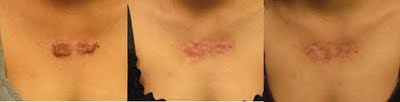
This patient had subtotal excision of a central chest keloid followed by radiation and then application of medicated tape. The photos were taken before, 1 1/2 months after and 1 year after surgery.
This patient also had subtotal excision of a central chest keloid followed by radiation and then application of medicated tape. The photos were taken before, 9 months after and 14 months after surgery.
In this case a burn scar of the face was camouflaged using follicular unit hairgrafts.
The ultimate goal, seldom achieved, is to hide a scar so that it is not visible to the unaided eye and the area in question looks as though nothing untoward has occurred. Scars never disappear and in many cases only a partial response is possible. The treatment of scars is usually not covered by health insurance unless a bodily function such as range of motion is affected or the scar is unstable. Some health insurance will cover scars from repaired injuries up to 1 year from the date of the injury.
Addendum March 12, 2012:
Neodyne Biosciences patented their Embrace Advance Scar Therapy system in 2010.
They received FDA approval in 2011. Just published studies on scars after abdominoplasty surgery show the system significantly improves the appearance of these scars. The system uses an applicator to stretch silicone tape which is then applied over the scar. The stretched tape contracts after application and protects the scar from tension and skin movement along the scar which would otherwise result in a bad scar. I cannot see the preferred use of this over regular medical tape which when properly applied can give the same kind of stress shielding at a fraction of the cost.
Addendum February 15, 2015:
A just published Dutch study of 29 keloids treated with injection of a freezing agent into the keloids followed for 1 year showed a 24% recurrence rate, loss of pigmentation in 69% of treated scars and an average 69% (range 16 to 100%) decrease in keloid volume. Some of these cases resulted in replacement of the keloid with a wide depressed scar containing abnormal looking skin. In conclusion intra-keloid freezing such as the CryoShape does not completely remove the keloid in all cases, is associated with a recurrence rate and can permanently whiten dark skin. It is not the gold standard in treating keloids.
Addendum July 1, 2015:
A review of 8 published studies on the use of intra-keloid cryotherapy revealed average scar volume decreases ranging from 51% to 63%, but no complete scar eradication was achieved on average. Scar recurrence ranged from 0% to 24%. Hypopigmentation after teatment was seen mostly in Fitzpatrick 4-6, darker, skin type patients. Finally, complaints of pain and itching decreased significantly in most studies. The evidence proved limited and inconsistent resulting in an American
Society of Plastic Surgeons grade C recommendation for this type of treatment of keloid scars. My conclusion is this treatment is best restricted to lighter skin patients who main complaint is pain and/or itching.
Lip Scar Revision
Keloid of the Face
Earlobe Keloids
Facial Keloids
Chest Keloids
Aaron Stone MD – Plastic Surgeon Los Angeles
Dr. Stone’s Twitter


![]()

![]()






Thank you for the article. I've suffered from keloids since the 1960's. None of the treatments have given me any relief. Now at 50 they hurt, itch & often deprive me of sleep. I may try the silicone sheets you mentioned. Again, thank you.
Thanks for the nice overview. Any particular reason why your patients haven't been happy with silicone based treatments?
my grandfather had a heart bypass surgery a couple of years ago (10 years approx) and the surgery resulted into a nasty looking keloid. also the keloid is painful upto this date. do you have cases like this? what could be causing this pain? its painful when touched. I would like to send you pictures if possible
Sure I would be happy to look at the photos.
Can you recommend a doctor to remove keloids in the midwest? I live in Cincinnati and L.A. is a bit far to travel to seek your analysis. I have two keloid scars and over the years realized that I am sensitive to keloid development. I had one treated with steroid injections, but the keloid was better for a month or two, but is now much worse. I have done nothing to the second keloid based on the success (or lack thereof) in treating the first keloid. Your suggestions are much appreciated.
I do not know anyone in your area but you can call the department of plastic surgery at your local university hospital and ask for a referral.
I see you worked at Wayne State University in MI, can you provide a recommendation in MI?
Dr. Kenneth Shaheen or Dr. Michael Busuito. Both are just north of Detroit.
Ive come accros your website and it seems that you can help me. Ive been searching for a long time for a surgeon who can fix my botched lip augmentation. If you can check out the 'blog' Ive put together and see if there is a way to fix this.
http://badlipaugmentation.blogspot.com
Thank you!
I had a patient with a similar problem. The silicone injection was fine until she had some dental surgery. When the dentist placed a tool to keep her mouth open during the procedure it shifted the silicone creating lumps in her lips. This presumably could have happened on its own over time due to lip movement. I was fortunately able to remove the lumps of silicone via small stab incisions placed inside the mouth. I would be happy to see you in the office as this approach might work for you.
i had a long ugly keloid resulted by a caesarian section 2years ago. i had it removed january 2010, waited for the wound to heal 2 weeks, then my surgeon performed laser treatment 10 times on me. unfortunately the keloid went back and its itchy and really getting me on my nerves. i am a filipina, light-brown in color. i have a cousin who also gave birth per c-section, who is quite darker than me, but she never had this nasty keloid like i do. i am currently residing in Germany and i dont have any idea now which and what treatment and where should i go for help.. maybe you could help me?
If you remove a keloid you can't leave a open wound. There cannot be any raw skin surface because having a raw skin surface dramatically increases the chances that the keloid will come back. That is very old school thinking to remove the keloid at all costs – it does not work. You are much better off debulking the keloid leaving enough surface skin to allow closure without tension or open wounds and then medically treating the area (pressure, injections or radiation) so the keloid does not come back. The treatment protocol you described having is associated with a high risk of recurrence as you have found out by now.
I have a long unsightly hypertrophic scar across the left side of my forehead which occurred as a result of injury in a car accident. This has had a major impact on my self-esteem and I have to cover it up with a fringe, which is really frustrating. What treatment would you recommend? Would complete removal in addition to radiation or corticosteroid injections help get rid of this thing from my face? Would a skin graft be an option?
What I would recommend would depend on what the scar currently looks like, what treatment you have had since the initial injury and the condition/laxity of the surrounding skin. I cannot therefore make specific recommendations for you without seeing you and knowing the history and current skin condition.
Most likely I would recommend cutting out the scar and starting fresh with a plan for preventing recurrence of a bad looking scar. That may involve scar taping, laser, scar injections, sunscreen etc. depending of the particulars of a given case.
Hi, my name is Angela i'm 17 I just stumbled upon your site. I got a keloid from having a cartilige peircing. I live in the D.C. area and I was wondering if you knew of any good surgeons that could assist me. Will the scar ever fully go away? Also, I was wondering if it was possible to get another keloid if I got a peircing somewhere else or a tattoo.
I am sorry but I do not know anyone in D.C. to recommend. There is no way to erase a scar. I can say that my keloid patients are happy with a flat soft scar that can easily be hidden by clothing or make up as compared to a protruding keloid that may cause symptoms like itching. Is is possible to get another keloid if you get another piercing. In fact I refuse to treat any ear keloid patients who plan to get another ear piercing.
Hi Dr. Stone, I am 19 and live maryland. About 3 years ago during a lacrosse game in high school, I was rushed to the emergency room because apparently there was a hole in my diaphragm. The operation was a successful but unfortunately I am left with a 6 in hypertrophic scar on my stomach. At first I thought it was because of the bad sutures that a scar developed so I recently got the scar excised the beginning of this year in january, but I think underestimated my recovery time and went to the gym too early. The scar came back and I was wondering could that be the cause of the recurrence, and if I got the scar excised again, what precautions should i take to ensure it will not come back? Thanks.
http://s28.photobucket.com/albums/c242/LoveNnadia/?action=view¤t=DSCN0538.jpg
Looking at your photo and reading your history it appears most likely that the scar is due to motion and tension along the suture line. To have a better looking scar it will need to be re-excised and then multiple modalities such as pressure, injections, medicated tape, laser etc. used to prevent a recurrence of the hypertrophy.
Hi, Dr. Stone. Have keloids on along my jawline as a result of acne. The keloids are around 2 years old. I'm just wondering if you successfully treated and flattened out the keloids of a patient whose keloids were 'specifically on the jawline' using silicone topical gel.
Also if it was successful, then how long did it take for the silicone to take effect (noticeable improvement)
Thanks.
I have successfully treated keloids along the jawline. In my experience the silicone gel or sheeting does not work in this setting. You need to surgically remove the keloids and then apply radiation or a combination of pressure and scar injections. I use a local company to make a clear mask that is held in place with velcro straps to apply the pressure.
Hi Dr.Stone,
First I would like to say that I appreciate your posting and the help you provide to others.
I suffer from keloid scarring on the back of my neck. They seem to be active (sometime they get flatter and sometimes the raise up a bit). I have had these keloids for over 10 yrs now and they are the result of bad acne from when I was a teen.
Do you think silicone treatment could help flatten the keloids permanently? If not, do you know of a way I can flatten it permanently?
Thanks in advance for your help
Never having seen your keloids I cannot make any specific recommendations. However, I can say that in my experience only applying silicone sheeting directly to keloids does not do anything to those keloids. The treatment is total or sub-total removal and then pressure and scar injections or radiation. The problem with a back of the neck keloid is the difficulty in applying any pressure around the neck for obvious reasons
I have Keloid scars in both ears. I was wondering what is the average cost for surgery and treatment for two similar sized scars
i recently had a keloid just below my knee removed. i used silicone tape on it for a while but i still have a somewhat raised scar as a result…its shaped like a horseshoe and it looks like i have a lucky charm on my leg. i try not to be vain about it but its so depressing. i just turned 18 and i live in Southern California, it would be awfully nice to be able to wear shorts again with no shame.
The cost of keloid treatment of the ears is dependent on the number and size of the keloids and which protocol option the patient chooses to prevent recurrence. If the radiation arm is chosen the cost of the radiation alone is $5000. If the scar injection with application of pressure option is chosen the total cost of this option is less but there are more office visits and the patient has to do more to get the desired result.
As for scars around the knee, these are very difficult to treat because of the amount of motion (in frequency and severity) normally present around these scars. Although I may treat a keloid in this area I would not treat any wide depressed scars or most hypertrophic scars around the knee as the failure rate is too high.
Hi may i ask how much is the price for this surgery . I have a lip scar just like that.i want to know the price of the one in your page.
https://aaronstonemd.com/images/scar-Revision.jpg
Hi may i ask how much is the price for this surgery . I have a lip scar just like that.i want to know the price of the one in your page.
https://aaronstonemd.com/images/scar-Revision.jpg
The cost is dependent on the type of treatment. Although 2 scars may look the same to the patient the treatment of the 2 scars may be very different due to scar location, surrounding skin laxity, scar maturity and other factors. These factors are obviously not all exactly the same in every patient, even those with similar scars. The cost could be as little as $1000 for an excision of a lip scar to $3000 for excision with tissue rearrangement like a Z-plasty. The cost also depends on the size of the scar.
Hi Aaron,
Great website, with some brilliant information on – thanks!
I was hoping you could answer a couple of quick questions for me please…?
Basically, about 4 years ago I had a crash on my motorcycle in the summer when I was only wearing a t-shirt and I fell along the ground and got bad road rash on my back/shoulders/knees and hip.
Some of the wounds on my shoulders and back turned into keloids whilst my knees and have healed (yes, there is a slight scar, but not keloidial…)
Here's some links to some pics of my scars for you to look at…
http://www.superstealthtrafficsystem.com/pics/Photo1.jpg
http://www.superstealthtrafficsystem.com/pics/Photo2.jpg
http://www.superstealthtrafficsystem.com/pics/Photo3.jpg
http://www.superstealthtrafficsystem.com/pics/Photo4.jpg
http://www.superstealthtrafficsystem.com/pics/Photo5.jpg
http://www.superstealthtrafficsystem.com/pics/Photo6.jpg
http://www.superstealthtrafficsystem.com/pics/Photo7.jpg
I was wondering, as knowledge of keloids here in the UK is not great what would the best treatment attempt be? (I finally realized what they were about 6 months ago and diagnosed myself – my doc didn't even know what they were!)
I was considering 2 options… Surgery with a proper surgeon who actually understands keloids (like yourself) or cryotheropy…
For a bit more info, I don't scar that easily usually, this is the first time I have encountered keloids – I'm 28 years old – was 24 when I had the accident.
And when I finally realized I these scars were keloids, I treated them with some black scar paste and SSKI – this has stopped ALL itching, growth, pain, etc and has really softened them and even flattened them ever so slightly in th past 6 months.
Sorry for the long question. I really do appreciate your time and look forward to hearing your expert opinion…
Kind regards
Rick
Cryotherapy does not offer any advantages over other treatment modalities. This is a very difficult area to treat because there is no loose skin around the scars (if you just cut them out and close the skin the closure is under a lot of tension) and the scars are in a very mobile area. These factors make the recurrence rate very high if you just cut them out and close the skin. You already know this because the scars here are much worse than scars elsewhere on your body due to the same accident. I suspect your best option would be to debulk the scars leaving some surface scar skin in place to allow tension free closure followed by some combination of irradiation, scar taping, scar injections and medicated tape to prevent recurrence.
Hi, I have a hypertrophic scar on my upper lip like the one in the second picture on your website https://aaronstonemd.com/ScarRevision.shtm except for maybe it's a tiny but thinner. How much would it cost to get it fixed? Would I have to go to California?
If it truly is like the second photo on the webpage you listed the cost for removal would be $800 to $1000 including a facility fee. If you wanted me to do the procedure you will have to come to California.
Hello Dr Aaron,
I have got some keloids on my left arm after a major burn from the lazer hair removal that took place since 3 months, that is in August.
I wonder if I can send you the phots and you give me your recommendations.
Is that possible?
Sure I would be happy to look at the photos but I will also need to know what treatments, ointments or creams were used to treat the burn.
Hi Dr. Stone,
Have you had experience or treat keloids with Bleomycin injections? There are numerous studies published that show to have positive effects on flattening and preventing recurrences. Specifically to it's anti-tumor properties of inhibiting fibroblast proliferation. I'm from Toronto, Canada, I am unable to find a doctors that is open to this alternative. Bleomycin seems to be practiced more so in India, South Africa, Korea, China where one would expect keloids to be more prevalent.
Thanks,
Antone
There are published reports documenting the efficacy of antitumor/immunosuppressive
agents such as 5-fluorouracil and bleomycin in treating and preventing keloids. There are more reports of 5-fluorouracil use in such a way than there are for bleomycin. I personally do not use them because of the significant risk of skin necrosis with an open wound that can scab over and take more time to heal.
Though they are not in my treatment protocols my patients still have had good results so I see no need to add them. The major difficulty is in treating recurrent keloids after treatment elsewhere by other physicians. These take more time and patience but I am willing to do that instead of adding anti-cancer medications to my treatment protocols.
Hello Dr. Stone,
I'd like to have a keloid removed from my left ear. I live in Riverside, CA but am willing to come to Los Angeles to have this procedure done by someone with experience in these procedures. What I'd like to do is send send you photos of the scar and get your initial opinion and suggestion for my best treatment options before scheduling an in office consultation. Thank You.
Hello Dion,
I would be happy to look at any photos you can email me. I can then reply with a detailed plan of action and cost quote. If all of that meets with your approval you can then see me in the office at a mutually convenient time and we can get this taken care of.
This is some great information. Thank you for sharing it. I have what I believe is a hypertrophic scar, raised and dark pink within the lines of what skin was cut out, on my left back shoulder from having a mole removed a year ago and having it cauterized. THis mole was not cancerous but the dermatologist was suspicous. This was how the dermatologist chose to do it, had i known this might have happened I would have insisted on him stitching it closed, but he didn't even mention that. It it still painful, rubs on shirts and bra straps and it is ugly. What would you suggest for treatment? Can this be cut out and stitched shut and not result in the same scarring? Would you go back to the same doctor seeing this was my initial result or try someone who may have more cosmetic experience? Thank you for your help!
Never having seen your scar and not knowing the amount of surrounding skin laxity I cannot make any specific recommendation in your case. This area of the body is well known for having little or no skin laxity. Therefore if you just cut out the scar you may not be able to suture the resulting wound closed or the tension on the scar line will be so great that the scar widens significantly over time. Therefore just cutting out the scar and suturing the wound closed is not likely to be a good option. Some degree of scar debulking, laser, scar injection and/or application of medicated tape for some months is more likely to be the best treatment plan.
Dr. Stone,
Thank you for providing such a thorough and informative posting. I have spent a lot of time researching scar revision and have found this most useful.
Approximately three years ago, I had a mole removed from my left shoulder. The scar that remained is somewhat wide and pink in color. That being said, my greatest discomfort with this are the track marks (look like railroad tracks) over the scar and have made me extremely self conscious.
I have tried laser treatments to try and minimize the appearance to no avail and would like to inquire as to what the best option is to remove the tracks or to revise this scar so that it is less visible? It is in a central area in which it is highly visible and I no longer wear short sleeve blouses as a result.
Please advise.
Best,
Rosie
If you could email me a photo of the scar and a more detailed description of skin repair and treatment after removal I may be able to help. Shoulder scars are notoriously difficult because of the constant tension applied to scars in this area. The skin hangs over the shoulders like a shirt on a hanger and that creates the skin surface tension.
Hello doctor! Ive had a keloid scar on my face for the past 4 years until recently i went to a beautician and i think she put acid on it causing it to burn and turn into a black scab and peeled off much earlier causing another keloid larger in surface area to grow back due to healthy skin being burnt. The keloid is slightly thick,red and right below my nose and slightly connected to the middle of my nose. What treatment would you recommend for the keloid? I would love to show you a picture if you dont mind. Thanks for reading.
Without seeing the scar I cannot be sure it is a pure keloid. I have to see it to know for sure but if it is a keloid it sounds like your best bet is excision followed by radiation and medicated tape to prevent recurrence. If just cut it out, burn it out or freeze it out it usually comes back worse and is harder to treat the next time around as it seems you have already found out. If it currently obstructs any portion of the nostril its treatment would be covered by health insurance.
I would be happy to look at a photo if you email it to me.
Dr. Stone,
Hello, I have a hole on the upper lining of my lip from horsing around with my younger brother. I was told it could possibly be a clogged pore but its to big to a pore and when i squeeze it nothing comes out. In the inside of my lip i feel a hard ball which i think is scar tissue. The whole is relatively small but very noticeable. Also the skin around it is darker than the rest of my face. Thanks for reading.
Without seeing a photo or doing a face to face examination I have no idea what this is or how to treat it.
Great post. I think it's wonderful that we have this technology nowadays. As a kid, I remember having friends/classmates who's got low self esteem because of the scars they got from accidents when they were younger.
Hi Dr. Stone,
I have a keloid on my left chest, and I am wondering if it would be ok to e-mail you a picture to see what kind of options you recommend as well as pricing? And are chest keloids more or less difficult to treat due to more tissues involved than let's say, the jawline or earlobe?
I was looking over your comments, and I am curious as to why options like cryotherapy or 5-fluorouracil use are not preferable to you due to scabs?
Also, in the pictures you've presented, the before and after was one year or less. Have there been higher recurrence rate after one year?
Thank you so much for your time and effort!
Thank you for submitting your excellent comment and questions.
Sure you can email me the photos by going to the contact me page or using the email button in the right column.
Chest keloids are difficult because there insufficient lax skin around them to allow complete excision and closure. Also the shape of the torso makes it very difficult to apply pressure to the scar after excision. So all of my patients with chest keloids have the radiation pathway of treatment after subtotal excision.
Cryotherapy as well as laser have no advantage over excision because it is what you do after excision that prevents them from coming back. If you just do cryotherapy or laser and nothing else they will all come back.
I do not use 5-FU out of personal preference. I have had such good results with medicated tape and kenalog injections without the risk of skin slough and scabbing that I do not see the need for adding 5-FU to my treatment regimen.
I have many patient photos going out past a year. Some a couple of years out. If the keloid comes back it usually does so within 2 or 3 months if no preventive measures are taken after excision. The key to proper care is knowing how and when to stop the preventive measures i.e. when they are no longer needed. That is different for every person and longer for recurrent keloids. Some recurrent keloid patients have to continue preventive measures for a year and a half while many first time ear keloid patients only need 2 or 3 months of preventive care.
Dear Dr. Stone,
As you have mentioned, the chest keloid is usually treated with radiation after excision. What are the possible risks after exposing radiation therapy?
Can I send you a picture to determine if they are keloids or hypertrophic scars?
Can you please suggest some doctors for keloid treatment in Northern California (San Francisco/San Jose etc.)?
Thank you very much!
That is better explained by the radiation doctor which they do prior to treating a patient. From my understanding the risks are minimal with the type of radiation used and the way they do it. I would be happy to look at the photos if you email them to me.
I had a bottle cut on my face,just below my eye,its a straight cut,it was sutured,after about 7 days the suture was removed and my doctor gave me kenalog injections so as to prevent keloid formation,its been a month nown,the scar has deepened and its looking darker than my skin and has widened considerably,but thats not my problem the problem is that am noticing small things like pimple growing out of there,when i try to press it nothing comes out of it,am realy worried if am begining to develop kiloid,and if so how can i prevent it as applying another kenelog injection will only make the scar deeper,pls i do realy need help on this as its got to do with my face and am a still a young girl i dont want kiloids growing on my face,any help will be highly appreciated.
Over injection of kenalog can result in wide depressed scars. If you could email me a photo of the scar I would be able to give you a more specific reply. You can find my email contact in the right column of this blog and on the contact page.
My mum has kiloids on her chest,another on her pelvic region,then two on her stomach,she resides in Nigeria,and wants to come to the US for the treatment,please can you give us an idea of how much this would cost and how long it would take and the best time to schedule this visit,and the neccesary steps to take to make this visit possible,she normally visits the United States regularly,any reply will be appreciated,thanks
If you email me photos of the keloid (you can find the email address in the right side column and the contact me page) I will reply with a plan for treatment and cost estimates.
Hi Dr.Stone,
I have a few keloids on my back shoulder blades just like the one in your first case photo. My sister has the same problem as well but she couldn't find any doctors that surgically remove keloids – they only suggested silicone sheets. Could you recommend any doctors in or around Toronto, Canada?
Sorry but I do not know anyone in Toronto.
Hi Dr. Stone,
My sister suffers keloid scar on her chest and shoulder for years. Can i see a pictures to see if you can perform a procedure to remove the keloid?
Thank You
What is your email address?
As you requested I have just added photos of chest keloids treated with surgery followed by radiation and then medicated tape. You can see that after a year the keloids have not returned and it is impossible to completely erase the scars.
Hi Dr. Stone,
What do you think about using 5-FU in combination with corticosteroids in treating hypertrophic scars? or keloids as well? I have a 3 y.o who just underwent craniofacial surgery and is developing scarring. His plastic surgeon is recommending this combo and I haven't seen much studies to support the benefits vs. the risks? What is your opinion based on your experience? Thank you for your time and help.
The 5-FU does work and there is clinical evidence for its efficacy. I have not found it necessary to add it to my treatment regimens. It has a tendency to kill the surface skin cells temporarily causing a scab which has steered me away from its use. Doctors who use it regularly may have better things to say about it.
hello Dr. stone i have the lump scar on my bottom lip and wanted to know which procedure would fix this and what kind of specialist would do this? i live about an hour and a half from Indianapolis,Indiana and wondered if you knew of any specialist in or aroud the area?
I have a small keloid on my left ear from a piercing i can still fit an earing in it but i choose not to. Its becoming an issue because its fairly visible. I'm afraid to cut it because it might grow back. Im only 18 and image is still important, after its removed ca i still wear earings? I have four holes in each ear but only this one has the keloid. Could it be from imprope care?
It could be from improper care but that is not the issue. The issue is if it is a keloid you have the genetic tendency and you need to let all piercings close because any of the other piercings can form a keloid at any time. The only earrings I would then recommend are the clip on kind.
My 11 yr old daughter has a very large keloid to her chest… tried kenalog, then surgical removal followed by silicone tape, multiple rounds of laser and keloid continues to grow at an exponential rate. What do you think of bleomycin tattoing?? have you tried it and if so what is your success rate?
In my experience silicone tape works well on hypertrophic scars but not on keloids, which you apparently have just discovered. I do not use the bleomycin because it has a tendency to kill the surface skin cells so the patient at least temporarily has a black scab.
Dr. Stone,
I have a hypertrophic scar on my chest where I had a mole removed as a teenager. It's not bad at all, an inch long and barely raised. I've wanted cosmetic surgery (facial) for some time. I know the chest is a fairly common place for hypertrophic scarring/keloids. My question is, does this disqualify me for plastic surgery? How can I know before undergoing a procedure?
Thank you
Based on your history you are not disqualified from cosmetic surgery but your surgeon needs to follow you more closely after surgery to ensure that you develop a favorable instead of an unfavorable scar. That means some office visits afterward for scar control with prophylactic scar injections, application of silicone sheeting etc.
Dear Dr. my name is Gill Nimrod Singh and i am from India . sir this year 6feb my body is burn and after the 1 and half month my body skin is become keloid and now my stomach,chest,arm,have big keloid i treatment with co2 laser 3 times but keloid never going, sir please tell me how to i make my skin before like skin because my age now only 24 years.i am very nervaus please tell me soluation about this.
thanks regards
Mr.Gill Nimrod Singh
(India )
gillsunny2010@gmail.com
Thanks for your article. I am currently 19 years old and I used to suffer from severe acne. I was put on a course of isotretinoin which helped to get rid of the acne but now I have a lot of very visible scars on my chest, back and shoulders. I just wanted to know if you think these scars are keloid or hypertrophic. They are dark purple in colour and bulge out of the skin with a shiny surface. They are still the same size as they were when they first appeared.
Without a face to face examination or photo I cannot say what they are. They could be either hypertrophic or keloid scar or a mixture of the two.
Thanks for your article. I had a burn scar on my breast about 1nch wide and 3inches long. It is flat but I want it smaller. What kind of surgery will I get and how much will it cost.
if you email me a photo I will be able to respond in greater detail. The optimal treatment would depend on the orientation of the scar and the laxity of the surrounding unscarred skin.
Hi Aaron, I have an itchy, big pink keloid scar on my ear lobe, due to a piercing close to the edge of my ear. All my ear piercings have turned into keloids, but the rest are tiny in size and white. The one I want to treat is pink and sore, here are some pics of it
http://pic20.picturetrail.com/VOL1358/13581698/24328753/406139220.jpg
http://pic20.picturetrail.com/VOL1358/13581698/24328753/406139221.jpg
I've had a course of 4 steroid injections, but they did not shrink it. Whats the best treatment available for this? I am from the UK, can you recommend any surgeons for me to contact? Thanks.
The best treatment is excision followed by pressure earrings and as needed injections.
Hi Dr Aaron
I had two moles removed on cheek and forehead by C02 laser 4 weeks back..the area is red and bumpy..i guess the laser settings were too high for my skin..i fear i might develop a hypertrophic scar or keloid..also the redness is not fading..should i go for any scar revision (laser or surgical)..or should i wait for few months..
Never having seen you and not knowing exactly what was done I cannot make specific comments. In general you want to keep new scars out of the sun for up to a year, sunscreen application will suffice. Also, it is easier to prevent a bad scar from occurring than it is to make a bad scar look better. Your original surgeon should be able to recommend specific prevention measures like scar taping, red laser etc.
hi..thak you for reply regarding co2 laser mole removal..as i said the moles are red and uneven..you can hav a look at picturs..
http://www.realself.com/question/red-uneven-scar-after-co2-lasr-mole-removal
should i go for scar revision or should i wait for few months..i'm applying sunscreen and silicon gel ointments..
It looks like the laser has removed most of the skin layers so I suspect you will eventually need to cut those scars out for the best looking result. However, you will have to wait a number of months till the scars have matured before knowing for sure. If the scars blanch when you press on them with your finger it is best to wait until the red color fades.
thank you. the skin layers do look missing like a 3rd degree burn. will the missing layers make me more susceptible to virus or bacteria..wound has healed but is there a chance of ulcer..do i need any extra care.. what is chance of getting back my normal skin after scar revision. if needed i would like to get it done at your clinic.
Some of the protective function of the skin is lost in those areas but that should not be a problem in normal daily use/exposure. These areas are not exposed to pressure like the walking surface of the feet so an ulcer is unlikely. There is no guarantee what the end result will be after scar removal and suture closure.
I have a hypertrophic scar on my nose from a piercing I had done… what would be the best treatment to get rid of it?
Never having seen you I cannot make any specific recommendations. The treatment options could range from fractional and flashlamp laser treatments with scar injections or medicated tape to excision of the scar followed by a protocol to prevent recurrence of a bad scar.
I have scar on my face plz.. tel me haw can I REMOVE THIS.
I looked at the photo on your google+ and honestly cannot see any visible scar such as a keloid or hypertrophic scar.
sir i have a post surgry scar on my neck…… plz help me out to remove this completly…. there was derma roller used on my neck but it leave lots of scar on my neck
If you come see me in my office I will be more than happy to help you anyway I can.
sir, i am from india…so its not possible to see you in your office….. i can mail my pic to u on your id…
Sure, email your photo to me.
Where can I get the medicated tape?
You can get it at any pharmacy including Walgreen's and CVS but you will need a prescription from a doctor before they will sell it to you.
What is the name of the prescription I should request for the medicated tape?
Cordran
Thank you for your post and replying to many people's comments. It has certainly helped me feel better about a friends scar which is only in its initial stages. Thanks again
sir i'm a 19 year old girl from Namibia. i wish oneday you will be able to help me as i have keloid scars on my face, mu tummy and my buttocks, i'm always crying and often people make fun of me. no boy even wants to date me because of this. i really hope sir oneday i could get the money and fly to your country. i can e-mail you my pictures if you want sir
I am very sad to hear your story. Unfortunately I do not have the resources to help you. If you can get to the capital city, Windhoek, I am sure there will be a doctor at the University of Namibia that can help you.
Hi I have a huge mole in the middle of my chest. My doctor recommended me to remove it because it is in a very odd shape and ugly but she did warn me that the chest area is prone to keloid. I have removed a few moles so far, one near my underarm and another waist. So far there is no keloid but it is dark in colour. Would you recommend me to remove it and through what kind of surgery to minimise scarring and so that the scar will not get bigger due to the lack of tension in the skin. Thanks so much!!
Never having seen you I cannot make any specific recommendation. If the mole only involves the superficial epidermal layers of the skin you might be able to remove it leaving the deeper dermis layer of skin intact and thereby minimizing the resulting scar.
Hello sir,
It is one of the best posts on keloids that I ever came across. Thank you very much for having shared such useful information on keloids.
Sir, I am 34 yr old female from india and have an about 1-1 and a 1/2 inch keloid on my chest. It had occurred spontaneously. I had no memories of its origin. It is almost 10 yrs old keloid. It is totally painless and causes no itching except at times when it is touched or massaged. The only problem is its ugliness n bulk. So, my question to you is whether I should go for its treatment or should I let it lie dormant…. Considering the fact that initiation of treatment might bring with it the associated pain, itchiness n other side effects and knowing that even after treatment, it won't go completely. Secondly, sir if I intend to go for the treatment, which is the best line of treatment:- (a) exicision followed by corticosteroid injections (b) debulking followed by corticosteroid injections (c) only corticosteroid injections (d)
corticosteroid injections in
combination with 5-FU.
Please help sir. If you advice, I can mail you the pics of my keloid.
Warm Regards
19
I cannot make any specific recommendations and I do not use 5-FU. I have successfully treated patients with what you describe using surgical excision/debulking followed by radiation or pressure, scar injections and medicated tape. Whether or not to proceed with treatment is up to you but if the surgeon does not employ a protocol to prevent recurrence it is better to forego any treatment of the keloid(s) by that surgeon.
Thanku sir. Please explain the exact difference between debulking and excision… N whichof these is a better/safer/more effective option ?
Please read my September 14 and March 11, 2010 replies for a better definition of debulking. Debulking is employed when excision is not a viable option in which case debulking becomes the better and safer option.
I have a keloid scar on my jawline due to cystic acne.
Do you do cortisone injections at your office? How much is the cost with and without insurance?
Never having seen you I cannot make any specific recommendations but I never just inject a keloid to make it go away. That does not work. Unfortunately there is no magic pill or injection that will make these scars go away.
Hi doc, I really admire and appreciate that you have taken time out of your busy schedule to answer questions here. thank you!
I also have a concern: a dime burn scar from a TCA peel 80% it has little hairs growing through it and occasionally I get pimples in the scar area which gives me hope that it can be remodeled. Am I correct in thinking this way? I live in Washington, DC and would like to know before visiting a plastic surgeon what would be your recommendations. Its flat l, hyperpigmented, and I'm African American. Thanks again
Oh the TCA burn is on my check bone very prominent when facing me.
I don't know the exact details of your treatment. Fom you description, if all you have is hyperpigmentation after an 80% TCA peel in an Afro-American you are lucky. I would expect something much worse. If you have active acne you need to see a dermatologist not a plastic surgeon. If you just want to lighten the treated area your best bet is a bleaching cream whose dose is titrated to give the the color you want or camouflage make up. Never having seen you I cannot be more specific.
Hello Dr. Stone,
Thank you for your posts on this topic. Very informative. Appreciate the effort you make in responding to questions.
I have a fairly large keloid scar (8 cm x 2 cm x 0.5 cm) on my central chest area for about 8 years now. It has evolved over time; becoming flatter in some areas but spreading over a wider area now. I can email you some pictures if you like.
The dermatologist advised me to do Kenalog-40 injections into the scar to help soften and flatten it. I understand that multiple sessions would likely be needed. I am worried of a recurrence of the scar. I have also read that injections also do cause the scar to "burn".
In your opinion, what would be the best line of treatment for this and to prevent recurrence? Would follow-up visits be needed to maintain the scar once it has "gone away"?
I cannot make specific recommendations without seeing you face to face or seeing photos with a complete history. In my experience kenalog injections alone do not treat keloids. The few people I have seen with very thick scars (not keloids) treated by kenalog injections alone, treated elsewhere, were left with thinned depigmented skin covered with telangiectasias and atrophy of the underlying fat.
I have had success with type of keloid you describe using a protocol of surgical debulking and either radiation + medicated tape or application of a pressure garment + medicated tape/kenalog injections +/- flashlamp laser.
The second approach, without radiation, requires frequent office visits over 8 months to a year and in the cases of recurrent keloids these visits may be needed for 18 or more months. After that maintenance visits are not required.
The radiation option requires less frequent office visits for 1 to 3 months after surgery but no maintenance visits after that.
Hi Dr Stone,
I've got a facial scar in my right side of my face from a car accident in August 5th 2012. I mean I think isn't that bad but it does makes me feel pretty uncomfortable when people stares at me. I would like to send some pictures about it, to see what would you do or recommend. I went to cosmetic place here in my city but all they said is I need DeepFX laser. But I think I need something else. Hopefully to hear from you soon Sr. Thanks!
Sure. Email the photos to me and I will respond with a possible plan of action.
Hi Dr Stone,
I have a 3.5 inches long and 0.25 inch wide scar on my right knee. It seems to be hypertrophic. Because of the location of the scar (right on the joint and horizontal straight), what would you recommend to minimize the scar? I've gone through 3 laser treatments but didn't help much. Would a scar revision help? If so, what kind? I appreciate your comments and if it's ok, I can send you some pictures of the scar. Thanks a lot!
Because the knee is so mobile in daily life surgical revisions of knee scars tend to be exercises in futility. If the scar is truly hypertrophic the best you can hope for is flattening of the scar through a combination of laser treatments, scar injections and/or medicated tape. In my experience most scars around the knee are wide, depressed and not amenable to revision.
You have had laser treatments but not all laser treatments are the same. The most helpful lasers for skin scars are fractional CO2 and flashlamp. The laser settings are also crucial as some settings will work while others can be of no benefit or even harmful.
I would be happy to look at your scar photos if you email them to me.
Hypertrophic scar on lip, same as the one on which you performed surgery- do you suggest dermabrasion
As of now there are no hypertrophic lip scar photos on this blog post. Dermabrasion is very old technology for scar treatment. It's drawbacks are it can't be used in individuals with darker skin colors, it is almost impossible to treat smaller scars without abrading normal adjacent skin and you cannot use it on non-skin mucosal surfaces. The fractional CO2 and flashlamp lasers do not have these problems. Excision and revision may be good options but in some people they are not good options because the excision results in a tension of closure that is so high it leads to hypertrophic scar recurrence. Without seeing you it is impossible for me to say what would be your best options.
Hi Doctor,
I have a very unique problem. I have BAD scarring on my areola due to constantly picking the little pores around my nipples. these scars have been there for as long as I could remember and it is very embarrassing. they are now like little black raised bumps that i am almost certain silicone gel CANNOT help. It may have to be cut out and stitched back or something. Can you help me?
I cannot make any specific recommendations without a face to face examination. If these scars are as small as you describe I do not think cutting them out is a good option as that would leave you with a larger scar. I suspect a fractional laser could be your best option but first you need to be diagnosed with a scar vs. other skin lesions. Sometimes the only way to make a diagnosis is looking at cells under the microscope.
Hi Aaron Stone its wonderful how helpful you are to people.
I have deep abdominal scars from surgery when I was few days born. I was throwing up everything I was eating so my papa said we must go to the doctor immediately so I had surgery in my gut stomach, it was 2 surgeries in the same place its about 3 inches long just above my belly button and few centimeters deep it doesn't look so horrible but very visible also,,, the 2 holes on the side so I could poop and the other to pie (those) got stitched up but it still looks like a hole from a distance.
Its like the lady in black sweater where the surgery connected the skin to the stomach muscles. Her surgery involved separating the deep from the superficial layers and a little bit of liposuction to even the surface contour. Let me know what do I need to make them look less visible like hers. I'd try to send pictures of my scars. Thank a lot
I can't say for sure without seeing you but it sounds like a similar procedure would help you.
I have a hypertrophic scar just on my upper lip, its pretty hideous, the doctor says that it can be cured by the Total Zcar FX, what are the risks involved? And if I do it, will my moustache hair grow again? Please reply.Thanks
There is no such thing as curing a scar. Anyone who tells you otherwise is not being truthful. You can only replace an unfavorable visible scar with a less visible more favorable scar. You cannot erase them.
Total FX is a fractional CO2 laser and there is no valid data that it is better than any other fractional CO2 laser. After multiple fractional CO2 laser treatments hypertrophic scars can be significantly flattened and softened but they will not be narrower, shorter or grow hair if they were devoid of hair prior to the laser treatments.
In the proper hands the risks are minimal and the worst that would happen is insufficient improvement in the scar. In untrained hands with inappropriate laser settings the scar could get worse.
Thankyou for your reply
Already have hair on that part, if laser is done on that part, will it remove the hair, and if it does, will that hair grow?
And I also have hair on an unwanted part under the scar, can that be treated?
The chances of a fractional CO2 laser killing hair follicles is remote. I don't know what you mean by unwanted part. Does that mean the initial repair or healing process did not properly align the tissues? If that is the case you need surgical revision, not a laser treatment.
Have a hypertrophic scar on my leg, how do I remove it?
Not knowing the history of your scar and never having seen it, I have no idea what should be done for it. In general the further down you leg the scar is the fewer options you have available for scar treatment because skin laxity diminishes as you approach the toes. The fractional CO2 laser and radiofrequency applied through pins have become the treatment of choice to flatten and soften most scars but they do not remove them. There is no way to erase a scar and the act of "removing" them in and of itself is a scar inducing process.
What does the CO2 laser do to the scar tissue?
The fractional CO2 punches microscopic holes in the scar with little reaction on the part of the skin so the scar flattens and softens but it is not erased.
Hello Dr. Stone
My teenage daughter had a surfing accident almost 2 years ago and the board hit the left side of her chin, leaving a long 2 in .scar that is raised and red in color. She is a model and very self conscious. We were given a topical cortisone cream but has done nothing, she has uses scar silicone patches as well but have seen no improvement. I was told to have her get cortisone injections and laser treatments. But I know they can be very pricey and being a military family on a budget will make it tough. What would your recommendation be.any advice would be must appreciated. Thank you for your time.
Never having examined her face to face I cannot make any specific recommendations. This area is very mobile, very visible and has very little adjacent skin laxity. These are the ingredients for a bad scar and then you add a teenager who is growing quickly and you have an even worse scar. Topical cortisone is of no value in treating scars so that is a waste of time and money. Cutting the scar out at this stage can also be a problem given the ingredients mentioned above. Your best bet is probably some combination of fractional and/or pulsed dye laser, scar injections and the application of pressure over the scar.
Dear Dr Stone
I have a big hypertroph scar on my lower arm since one year (burns). Now I have noticed, that pores (and hairs) are coming through the scar. Some of the pores are darker than the others. When i squish these pores, a string of white stuff comes out. Can you tell me, what do these pores mean? Does it mean that the scar is healing and flattening (there is no visual improvement)? Should i stop squishing them or is it good to do so?
Thanks alot already
Rachel
Enlarged skin pores are common after more superficial burns. What you are describing is the equivalent of a blackhead or comedone. Shed surface skin cells (Keratin) combine with skin oil to block the pore. Oxygen in the air interacts with the material and darkens it. Touching and picking at them might cause irritation, infection and more hypertrophy of the scar. Washing or scrubbing the skin too much could make it worse, by irritating the skin.
The best way to clean out the pores is a Comedone extractor. Be sure to cleanse the area of skin with warm water before and after and to cleanse the extractor after each use. Also do not use the sharp end on yourself.
Hello Dr. Stone, my 3-yr-old daughter had a lip injury that has left her with a misalignment of her vermilion border (it was pushed up in one spot by one of the sutures and then it steps off), there are also white scars on the red part of the lip from the sutures, and some scar tissue when has distorted the overall lip shape. We have consulted with a few of plastic surgeons so far and two said to go ahead and do the surgery now because she's young and will heal better at this age while two suggested waiting until she's done growing and also at this age, because kids heal so quickly, she will be more prone to scar tissue formation. Also, I'm a bit confused on the method because one said he would do a z-plasty, one said a vertical incision (which means shrinking the length of the lip on that side), one said to do a diamond shaped cut, and the other said to do a horizontal incision and try to place the scar along the white roll of the lip. Anyway, I'm a bit confused and I don't want to drag my daughter to many more consults. Do you suggest doing something now or waiting until she's a teenager? I have thought about getting a medical grade tattoo as a temporary solution to try to camouflage the area a bit but I'm not sure if that would interfere/cloud the visibility for a surgery if we do move forward with it. Any advice would be much appreciated. Thanks so much!
Whatever you do don't tattoo her. It will only make things worse. As for timing at this point it does not matter when you do it as long as it's a year plus out and before she becomes conscious that there is something wrong. As to technique of repair I cannot be specific as I have never examined her and do not have a complete history but can make general statements. Different surgeons can use different techniques and still achieve equivalent results. Z-plasty is what we were taught in residency but that modality does not seem practical to me. My personal preference is usually to remove any widened scar, recreate the original injury and then realign the tissue for the repair. You have to place a temporary tattoo in the skin first in order to do the alignment because once you start injecting and cutting everything becomes distorted. This should all of course be done under magnification.
i have a hypertrophic scar as being said by one of the doctors. He said that ill need to undergo CO2 laser to remove it. Do i have to shave the hair off before the laser?
You should always shave hair before a laser treatment of the hair bearing skin. Otherwise the hair will absorb the laser that was meant for the skin.
Is there anyway in which i dont have to shave it and theres no damage to the hair either
No there is not.
Hello Mr.Aaron,i have a wide scar on my lip, should i prefer laser over surgery or vice versa
Never having seen or examined your scar and not knowing the history of the scar it is impossible for me to give you specific answers. In general lasers are not so good for wide depressed scars and surgery only works for widened scars that have sufficient surrounding skin laxity to prevent recurrent widening.
Hello Dr. Stone,
I am so pleased to have stumbled upon your blog! It is so informative and helpful and so I thank you for that.
I am a 19 year old Filipino and am currently suffering from 3 rather small keloids on the center of my chest about an inch or so below my clavicles (the largest/oldest of the three being about 1 1/2 cm in diameter). Keloids are genetic since my older sister has one on her shoulder from a vaccine shot when she was little, and my little brother has one near his elbow caused by a bike fall. My keloids started to develop I believe sometime near the end of 2013 because of acne; however, I didn't know they were keloids at the time until around June of 2014 when I visited my dermatologist (not for my keloids but for my facial acne) and asked about what was on my chest. That was when she revealed to me that they were keloids. That day the resident dermatologist, with the permission of the head dermatologist, treated all three keloids by injecting a corticosteroid. The next month I returned to the dermatologist for a chemical peel as well as injections for some of my acne but also for my keloids. I believe they used the same dosage of the steroid used for my acne also for my keloids so I'm guessing the dosage was quite low. After another appointment and getting my keloids injected again I discontinued because I didn't see any changes, it was extremely painful, and because I felt like the dose was too low and that the injections only caused the keloids to get bigger when the keloids were healing.
I feel like there isn't enough skin for complete cutting of my keloids but I think there is enough to debulk my largest keloid which is protruding about 1/2 a centimer or so above the normal surface of my skin. Another question, when you treat your patients' keloids and use kenalog, do you usually numb the area so that it won't be so painful? What do you do with the keloid right after injecting it? The resident dermatologist I had put a bandaid on my keloids right after injecting them but then the nurse who injected my keloids at my last two appointments didn't use anything after injecting my keloids so I don't know what the best thing to do. Also, are there any side effects (short and long term) when using the radiation? And is the surgery to cut/remove (or just debulk) and radiation expensive or covered by most insurances?
I'm sorry for bombarding you with all these questions but I am very eager to have my keloids flattened but it's hard to find a dermatologist with keloid experience like yourself. I found that you have recommendations for doctors in Michigan but I don't know if they will accept my insurance.
May I send you pictures of my keloids? I have pictures of them over the course of about 1-2 years (i.e. when they still looked like acne back in '13, when they were injected, till now where it's more protruded and red).
Also, could you look over this post I found about a woman's journey of how she had her chest keloid flattened? My keloids are definitely not that big or wide like hers but I would love to know your input on how her dermatologist treated her keloids and if you agree with it/recommend it for myself. Her doctor is Dr. Gary White from Kaiser Permanente in San Diego.
(http://thoughtcatalog.com/vicky-oppenheim/2013/05/my-treatment-for-keloids/)
Again thank you so much Dr. Stone for your blog and for your responses to these other commenters as well. Hope to hear from you soon! Please let me if I may email you the pictures. Have a blessed day!
Thank you for reading my blog and posting your wonderful comment.
Doctors familiar with keloids know that a 10mg/cc solution of kenalog will have about as much effect on a keloid as bullet does on superman. For most central chest keloids I prefer a combination approach of surgical debulking, radiation and medicated tape. This protocol deals with removal and effectively prevents recurrence. The use of a multimodality approach diminishes the risks associated with just one modality if you use too much of it. Just injecting steroids is not my first choice because the injected particulate material can be found under the skin for the rest of your life and in darker skinned individuals can cause permanent depigmentation in the normal skin around the keloid. The current problem with the approach is that the tape has gone from $30 to $40 before Obamacare to over $300 after Obamacare. The radiation is not recommended for younger patients and I have seen radiation burns when outdated equipment is used or the radiation doctor is not that good.
There are multiple new approaches out there like liquid nitrogen injection and application of medicine laden sheets with multiple tiny needles that address keloid removal but then you still have to stop them from coming back.
In most cases insurance does not cover the treatment of keloids.
Patients with keloids need to be very careful if they are undergoing any procedure that can damage the skin including chemical peels, laser treatments, tattoos, surgery etc. because any of these can cause another keloid.
I would be happy to review photos of your keloids.
Thank you Dr. Stone for taking your time in reading and responding to my post! Also, thank you for making your response thorough and easy to understand. I will be sending you photos as soon as I can!
Hello Dr. Stone,
I have had a Keloid behind my left earlobe for over a year now. At first before I knew what it was and while it was still small I continued to wear earrings and since I am a college wrestler I continued to wrestle without headgear. It grew exponentially during this time and now it is about the size of a small grape and is really tender to even touch. I no longer wear earrings or plan to wear earrings anymore in either ear and always wear my headgear but it is still very bothersome. I read on a forum that putting tea tree oil on it sometimes helps and so I have been applying it to the keloid for the last few months and I feel like it has become worse.
I was wondering if I could e-mail you some pictures of it and if you have any recommendations on any procedures to help either remove it or subside the pain as well as general pricing for the procedures.
Thank you for your time.
Earlobe keloids are the easiest keloids to treat because you can apply pressure to the ear lobe after keloid removal more easily than to any other area of the body. Historically pressure earrings were used. Some years ago small acrylic plates became available which are much better. The plates are held in place with small screws so you can make minute changes in the applied pressure. The plates are clear so you can always see the underlying skin and make timely therapeutic adjustments as needed.
I would happy to look at the photos if you email them to me.
Hi Dr Stone,
Im not sure if my first comment posted but Ill try again. I want to know your opinion on this scar that ive had for the past 10 years. Im not sure what kind of scar it is but ill describe it. Its dark and a bit raised. It does not have a smooth texture. I have tried TCA peels where the first 3 sessions nearly cleared the scar completely but I over did it and the scar came back to the same size,color,texture.I also did lactic acid peels where it also nearly faded the scar completely until i also over did it and the scar came back.When I initially started using Retin A, it actually smoothed out the scar and nearly faded it but I picked the skin too early and the scar came back. All of this happened a couple years ago. I went to a derm and her gave me Tri Luma. All it does at this point is lighten the scar but it doesnt improve texture of flatten it completely. I dont think the scar is completely healed either since the peeled skin just reveals red skin underneath then it heals right back to the dark color and bad texture. I want to know what you think before i consult a plastic surgeon. I have added some pics to help.
http://i61.tinypic.com/20fqiwy_th.jpg
http://oi59.tinypic.com/2r5cl6q.jpg
Sorry but your photos are not optimal for assessing the scar(s). Currently the best way to flatten and soften a scar is fractional CO2 and flashlamp laser treatments. I don't know if those treatments should be performed on you given the limited information I have on your case. I don't see any role for chemical peels or retinA in treating raised hard scars. Also, I am not sure I would want to treat someone who has had multiple mistreatments for scarring and picks at their scars. The odds are stacked against a good result.
Thanks for the reply
To be more clear. The scar isnt hard, its actually quite soft. Its slightly raised but the texture isnt smooth. If I can describe it better, when i went to the derm, he thought it was melasma at first. It looks more like hyperpigmentation. The retin a does lighten the scar but the issue im having is that the scar doesnt completely flatten or fade into the rest of my skin tone.
To explain the chemical peels that were done. The peels worked in the beginning but I got over zealous and picked off the peeling skin too early. I wasnt necessarily picking at the scar itself but the peeling skin.
I got the scar as a result of acne. If that helps
Sorry but that does not help and the answer is still the same. The treatment applies to raised scars regardless of how hard or soft you think they are.
Hello Doctor Stone,
Reading the whole article made boost my confidence that my old scar can be treated. I have a scar on my upper lips same as the picture above with the girl having a wedge scar on her upper lips but mine is lesser and not noticeable but almost the same appearance. I has been bitten me accidentally and had 4 stitches and it leave a bump as what I mention above. How long it taste to be healed? Thank you very much.
From what you described it is healed but not yet mature. The question is what will it look like after it is mature and can you do anything now so it will look better once fully matured. Without further details and examination I cannot answer that question.
Good day, Doctor Stone.
Glad that I able to find your blog here about scars. 7 years ago, my dog accidentally bitten my lips when we were playing and cuddling each other. I was been rushed into the hospital and stitches my upper lip, after two weeks, the doctor removed the stitch when the wound healed totally there were small bump left I don't know if it is a keloid scar but It doesn't hurt when you pinch or touch it and has a same color and appearance like my lip color. Actually its not that noticeable but when you sight it near it really has a bump like an ant bitten my lip or just like a mosquito bite bump on my upper lip. The scar is not hard Its a soft bump on my lip but I want to remove it because It is one of my biggest insecurity on my body for years now. Thank you very much Doctor Stone.
You will need to see a doctor to know more certainly but it sounds like a case for laser treatments.
Hello Dr Stone,
I got bit my a dog on my lip which I have small bump on my upper lip.. It leave a small bump which isn't that noticeable which i guess its not a keloid because it isn't hard when you touch or feel it.. Can this bump on my lip will remove? Actually it has the same appearance and color of my lips but when you zoom and look closely you will notice a tiny bump like I was been bitten by an ant. Is there any way that it can be remove? Thank you very much!
Sure it can be removed but there is no way for me to know if that is your best option without a face to face examination. Fractional CO2 may be a better option but there is no way for me to know that with the little information in your comment.
Good day Dr. Stone. I had stitches removed from my upper lip 10 years ago due to dog bite. Underneath the upper lip there is a lump of tissue that protrudes out from under my lip that when I touch it there's like a jelly bean inside. Is it possible to get that extra tissue removed?
I went to a derma but she suggested to inject it a steriod but I am afraid of the side effects or it will change the appearance of the scar. Or is there another way to remove the scar?
Thank you Dr Stone.
Hi,
I got my keloid remove, two years ago, but it grew back, one reason i think it grew back because i do Brazilian jiu jitsu. I'm just remove it a second time, i was wondering if it would help if i wear a headgear when i do Brazilian jiu jitsu? Thanks
I assume you are referring to your ears. In BJJ this is usually due to blood collections or hematomas under the skin and is called a cauliflower ear. It is not a keloid though it may look like one to a lay person. As long as you do BJJ your are susceptible to cauliflower ear. Head gear will prevent it by preventing direct trauma to the ears. Without a face to face exam or photos I cannot say for sure what you have.
I have injury scared and damage upper lip very similar to the firs photo by article. The insurance will cover because this damage raise from prior accident. I have difficulty in finding skilled doctor.
The car insurance could cover it if the limits of the policy have not been reached. Health insurance might cover it, it depends on the wording of your policy… If you come see me in the office I should be able to tell you whether I might be able to help you.
hello doc,
I have suffered with keloids on my earlobes since I was 12 and have had 9 operations to remove them and of course, they keep coming back. I am afraid that I have been taking the kenalog injections to long and wonder if there is any side effects. Also , I tried wearing the pressure earrings but they cause severe pain after a couple of days and make the keloid reappear when they were once flat. I stop wearing them. However, I wanted your feedback on tummy tuck keloid scars. D you think it is possible for it to occur because I am considering having the procedure.
Given your history of recurrent keloids you are at high risk of forming a kelid scar after tummy tuck surgery. As you have realized surgery alone does not cure keloids. It is the care after surgery to prevent recurrence that is the cure. The major complication of kenalog injections are thinning and depigmentation of the skin. The pressure earrings are old technology. The current method of pressure application is clear acrylic plates placed on each side of the ear that are held together by acrylic screws. This allows fine adjustments in the amount of pressure applied to the ear so pain is less likely. Given your likely reticence to try the surgery pressure treatment of the ear your only other option would be surgery and radiation to prevent recurrence. Your best bet would be surgery for the keloids and tummy tuck at the same time with application of the plates to the ears after surgery and cordran medicated tape or haelan cream+tape to the tummy tuck scar beginning right after tummy tuck skin suture removal. At the earliest sign of increased metabolic activity of the tummy tuck scar flashlamp laser treatments would be helpful. You may have to apply the medicated tape for as long as 12 to 18 months. This regimen should help treat your current keloid and prevent keloid formation at other surgery scars.