Body dysmorphic disorder (BDD) is a syndrome characterized by a strong preoccupation with an imagined defect in a person’s appearance. In cases where the deficit is not imagined and a slight defect is present, the person’s concern is noticeably excessive. Excessive preoccupation with the imagined or minor flaw involves intrusive thoughts about the body part of concern. In addition to daily intrusive thinking, individuals suffering from BDD engage in a variety of compulsive behaviors aimed at alleviating the anxiety caused by the thoughts.
Patients with BDD generally engage in thoughts and behaviors related to their perceived deficit for 1 hour or more per day, and that amount has been reported as high as 3 hours per day among adolescents. Symptoms often start in adolescence or early adulthood brought on by remarks made by peers or family members i.e. early bullying and family attachments are significant factors. The average age of
onset is 16 to17 years, although it may occur in older adults overly concerned with their aging appearance. Individuals with BDD frequently check their appearance in mirrors to confirm or
attempt to conceal the perceived deformity. They may engage in long rituals of grooming, such as repeatedly combing or cutting their hair to make it just so, applying make-up, or picking at their skin. They typically will spend a great amount of time trying to cover up or camouflage the perceived defect employing elaborate clothing rituals. They will seek excessive reassurance from friends, family members, and/or co-workers to elicit placation that the perceived “defect” does in fact
exist, or to assure that the flaw is sufficiently concealed. At the extreme they feel anxious around others, avoid social situations, become housebound, only leaving their homes at night to avoid the scrutiny of others. Some drop out of school, avoid job interviews, or do not work in order to avoid
public exposure . Patients with BDD have attempted to engage in self-surgery with knives or razor blades to pick at or remove the blemish or with staples to tighten “loose skin”. Clearly they see something that others do not see real, imagined or exaggerated.
Since the rise of smart cellphones, social media and reality television promoting narcissistic behavior the majority of BDD patients have a compulsion to repeatedly take and post selfies on social media sites. They might take several selfies over and over again until they find the right one. Picking out details about their eyebrows, skin, noses, smiles, teeth, hair and so forth, all in an attempt to find the perfect angle to make the perfect picture. As harmless as these acts all seem, they build up over time to create great forms of self consciousness and false sense of confidence feeding on itself as an ever growing consuming obsession and compulsion. Instead of being okay with who they are no matter what, they strive to find the right picture with all the perfect details. The more likes they get on social media sites the happier they feel. Narcissism, being obsessed with receiving recognition and gratification from ones looks, vanity and in an egotistical manner, is becoming a big problem in our digital age. A recent survey showed that 16-25 year olds spend on average 16 minutes and seven attempts to take the perfect selfie.
Danny Bowman, a British teenager, became so obsessed with capturing the perfect shot that he would spend roughly 10 hours per day taking up to 200 selfies trying to get the perfect shot. As things got more and more intense for Danny, he lost nearly 30 pounds, dropped out of school and did not leave the house for six months as he kept trying for the perfect picture. He attempted to commit suicide because he was unable to take what he felt was the perfect selfie but the attempt was thwarted by his mother. He stated that he “was constantly in search of taking the perfect selfie and when I realized I couldn’t, I wanted to die. I lost my friends, my education, my health and almost my life.” 40% of BDD sufferers experience suicidal ideation at some point throughout the course of their illness.
Concerns with weight fall into a separate eating disorder classification. BDD can manifest as eating disorders, obsessions with exercise and fitness and addiction to plastic surgery though the Diagnostic Statistics Manual considers them separate entities for descriptive usefulness. Even the rich and famous can be affected. Former British glamor model, Alicia Douvall, who associated with music mogul Simon Cowel and was linked to actor Mickey Rourke and Simply Red singer Mick Hucknall spent over £1m on over 300 procedures. At one point she underwent one operation a week because she was convinced that she was ugly.
Yet in 2013 she turned on her plastic surgeons saying they never refused her even when she brought a Barbie doll with her to illustrate what she wanted to look like.
Looking at Michael Jackson over the years as he gained then lost his nasal bridge, his wide base narrowed then collapsed and his implant began to protrude through the tip it is obvious that he was the text book definition of BDD.
27 year old actor Reid Ewing on the show Modern Family began having surgery at the age of 19 in 2008. Starting with cheek and then chin implants he continued to have problems with surgery requiring another operation to fix the previous operation. He also had a history of eating disorders but the subject was never broached and he was never referred for psychiatric evaluation by any of the surgeons that operated on him.
A Baltimore man showed up in his surgeon’s office in a trench coat after rhinoplasty surgery. He threatened to shoot himself and others because he said his nose was not quite what he wanted though there is no evidence there was anything actually wrong with his nose after srugery. Police we called to defuse the situation and it fortunately turned out that he was not armed.
A man in his early twenties once came to see me in consultation for a rhinoplasty. His avoidance behaviors and exaggerated reactions to my physical findings were a red flag. I told him it was my policy to send males in his age group for this surgery for evaluation by a psychologist. Luckily, I had another patient who was a psychologist specializing in BDD. To my surprise a phone call corroborated the diagnosis of severe BDD with suicidal tendencies, and avoidance of socialization by not working and spending most of his time at home where he was cared for and medicated by his physician parents. I was warned not to operate on him no matter what. Another female patient was overly concerned about her facial bones and her urgency in obtaining surgery for non-existent deformities was alarming. I sent her to the same psychologist who told me that she did not have BDD which surprised me even more than the assessment of the man in his twenties. Needless to say I refused to perform surgery on both of these patients.
In light of the risks and harms cosmetic surgery can cause patients with BDD, having a systematic process for identifying such patients is imperative. A study published in January 2015 described a screening questionnaire using utilized the Body Dysmorphic Disorder questionnaire (BBDQ) and the Body Dysmorphic Disorder Structured Clinical Interview for DSM-IV (BBD SCID) in 234 patients presenting for facial plastic surgery for this purpose. They confirmed a diagnosis of BDD in 13.1% patients undergoing cosmetic surgery and in 1.8% of those undergoing reconstruction surgery. The incidence in the general population is estimated to be 2%. The BDDQ was determined to be 91.7% accurate, 100% sensitive and 90.3% accurate in screening patients for BDD, according to the researchers.
In patients with BDD, the nose was determined to be of most concern (56%), followed by the skin (28%), hair (6%), chin (6%) and ears (6%). Those with markedly excessive concern over their noses report distress regarding its size or shape.
Concerns with the skin typically involve acne, wrinkles, and spots. Thinning and balding are usually the main concerns reported among individuals preoccupied by their hair. Patients with BDD were found to have elevated depression levels compared with patients without BDD. This explains why Michael Jackson had more nose surgery than any other surgery.
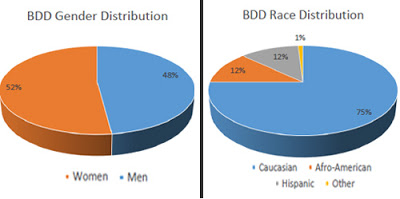
Other epidemiologic studies have shown
52% are women, 75% are Caucasian, 12% are Afro-American and 12% are Hispanic.
Three out of 4 people with BDD are unmarried; however, women with the disorder are more likely to be
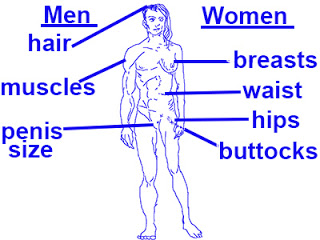
married and men more likely to be single.Women are frequently troubled with their overall weight and the size of their hips, waist and breasts; men are more distressed about their height, genitals, penis size and hair. Men are also more likely to exhibit a specific type of BDD, referred to as
muscle dysmorphia, a preoccupation with being too skinny and lacking enough muscle that leads to anabolic steroid use.
Over the last decade buttock size has been a major focus for a variety of reasons. Leading to multiple deaths and deformities (see my blog Brazilian Butt Lift).
Most patients are concerned with more than one body part at a time especially those obsessed with exercise, fitness and muscle size. In fact, the average BDD sufferer is concerned with three to four features at once.The overall prevalence of BDD in the U.S. population is 2.4%, but the incidence is significantly higher within the cosmetic surgery population. Among cosmetic surgery patients, the reported prevalence rates range from 2% to 7%, and the rates range from 9% to 15% among dermatology
patients. Thus the prevalence of BDD among the overall aesthetic patient population may be up to 7 times higher than in the general population.
Although BDD is treatable most people with BDD delay seeking help for fear of being dismissed as vain. The earlier it is diagnosed, before the thoughts and anxieties have become fully ingrained, the easier it is to treat. Treatment consists of a combination of an anti-depressant medication and cognitive behavioral therapy with a psychologist/psychiatrist before and after, or instead of a cosmetic procedure.Cognitive therapy teaches patients to identify unhelpful thought patterns and replace them with more constructive ones, control anxiety and obsessional rituals, increase self esteem and feel more comfortable in social situations. It does not focus on the cause of BDD. It can take several months for the treatment to take effect. The minimum treatment duration is 2 to 3 years and medication may need to be taken for life to prevent relapse. Psychoanalysis is time consuming, expensive and an unproven treatment for BDD. The BDD sufferer on the other hand is convinced surgical or medical treatment is necessary and psychological treatment will not resolve their problems. While delaying appropriate treatment the BDD sufferer may try to cure themselves with plastic surgery but only 10% of those who do will be happy with the result of their surgery. Hence the propensity for them to have multiple procedures. Sadly in today’s world if you look hard enough, you will find someone who will do almost whatever surgery you want. A large number of those who undergo plastic surgery experience a worsening of their BDD symptoms, while others may develop a preoccupation with another body part.
Studies have consistently demonstrated that the majority of people with BDD do not benefit from cosmetic treatment.
Family members of someone with BDD should:
- avoid debating the existence of the perceived defect because that can entrench the delusion
- set boundaries such as being alone in bathroom time
- avoid contributing or condoning rituals or avoidance behaviors such as making excuses to employers or providing camouflage materials
- not supply money for cosmetic surgery because the surgery will not solve the problem
- encourage treatment by a psychologist or psychiatrist specializing in BDD because it is highly unlikely they will initiate appropriate treatment on their own
Addendum December 1, 2015:
A 34 yer old Russsian recently discharged from the Navy presumably with post traumatic stress disorder had multiple rhinoplasty operations beginning in 2010. After his last nasal surgery in St. Petersburg he told nothing more could be done and the assistant chief of surgery, who did not operate on him, sent him a letter advising that he undergo psychiatric care. He returned to the hospital with a Vepr machine gun and killed that doctor and then himself. This is a classical tragic ending to someone who under went surgery for BDD.
Dr. Aaron Stone – Plastic Surgeon Los Angeles
Dr. Stone’s Twitter












Join the Discussion!