Steroids refers to a broad group of chemicals produced by the body and drugs or medications with a spectrum of properties. All steroids have a common 4 ring chemical structure with side attachments that change its name and properties giving rise to everything from testosterone to bile, estrogen, estradiol, progesterone, prednisone, decadron etc. Most of these are found in nature produced by animals or plants but some can only be made synthetically in a lab. There are 2 main categories sex hormones and corticosteroids with subcategories that apply to each.
Their relative category potencies and time length of effect vary. Dexamethasone’s glucorticoid effect is 80 times stronger than cortisol, it lasts 6 times as long and has no mineralocorticoid effect. Testosterone is 5 times stronger than androstenedione. As the doseage or blood level increases each chemical begins to have effects in other categories so a high doseage of prednisone can start to cause water retention, a mineralocorticoid effect.
This blog post will focus on the glucorticoid portion of the above table. Glucocorticoids are commonly prescribed for allergies, asthma, a variety of skin conditions, ulcerative colitis, lupus, arthritis and many other different diseases as well as after transplant surgery. In the UK in 2008 0.79% of the population was prescribed long-term (i.e. ≥3 months) oral glucocorticoids. That is 484,270 people. In 2016 glucocorticoids were the 19th and 49th most common prescriptions in the US. In 2017 prednisone was the third most common prescription in the US.
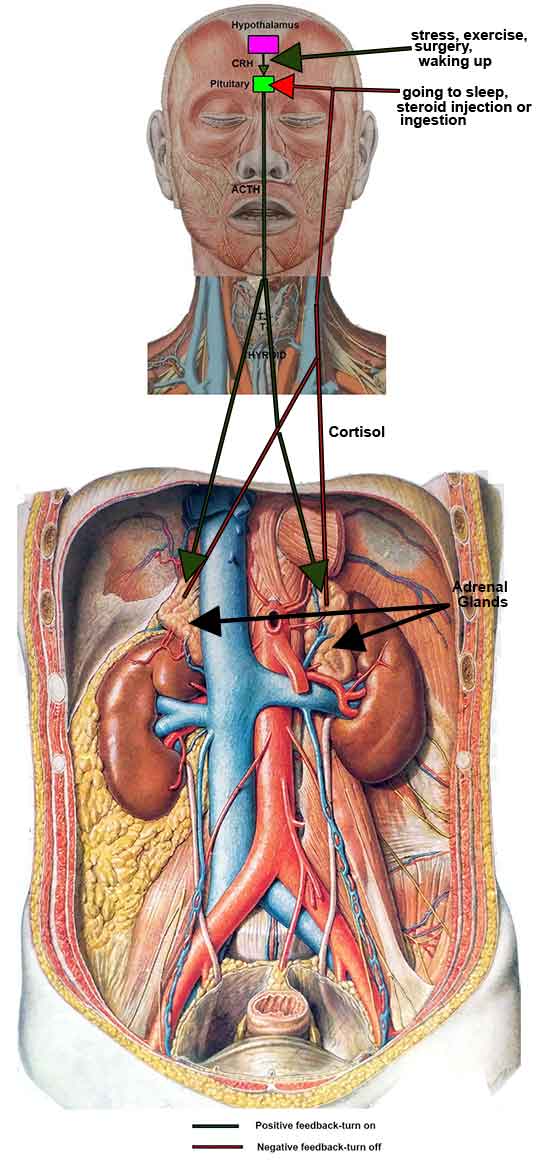
Glucocorticoid production by the body is regulated through feedback mechanisms via the brain (hypothalamus and pituitary gland) and the adrenal glands that varies with emotional states, sleep wake cycles, fasting vs. eating and activity levels. The brain stimulates the adrenal glands and high adrenal output reduces brain stimulation. The stress of surgery causes cortisol levels to rise within 45 minutes of skin incision, peak 5 to 10 times normal within 10 hours after surgery and fall back to normal within 24 hours if all goes well. The brain adrenal axis of control is primed to the equivalent of about 7.5mg prednisone per day stress free baseline. At lower levels the brain signals the adrenal glands to produce more. Therefore, medication doseages higher than this turn the axis off and make it less responsive or sensitive to stresses. At the extremes of low body production (Addison’s disease) and high body production (Cushing’s disease) there are easily visible body changes. In between those extremes the levels can still be such that response to surgery is impaired despite there being no visible physical indication before surgery because the brain adrenal control axis is impaired. This was first noted in the early 1950s in patients who had been taking glucocorticoid medications before surgery and collapsed after surgery with low blood pressure that normalized after the patients were given glucocorticoids. Thus there are 2 factors to consider, the baseline level of these chemicals in the bloodstream and the ability of the brain adrenal axis to respond to stress. The blood levels can be abnormal due to internal body causes such as adrenal failure or externally ingested or injected medications such as prednisone. Furthermore, different individual’s bodies respond differently to the same doseage of these medications depending on the length of time of exposure. Once the brain adrenal axis has been exposed to the equivalent of about 7.5mg prednisone per day for as few as 5 to 7 days it takes up to a year without exposure to the medication for the adrenal portion of the axis to regain its sensitivity to brain stimulation. So even if the unstressed blood levels are normal within that time period the adrenal glands can’t secrete more when stressed and can result in collapse. In such patients the recommendation is IV injection of 100mg of hydrocortisone (25mg of prednisone or 3 to 4mg dexamethasone) at the beginning of surgery. For minor surgery or imaging procedures with dye that should suffice. For more extensive surgery or complications following surgery the medication is given every 8 hours for 24 or more hours.
For safety in cosmetic surgery these patients have to be placed in 2 groups. The first is that which is not currently taking glucocorticoids but has an impaired brain adrenal axis. The second is that which is currently taking glucocorticoids for a chronic disease. The first group is treated as described above. For the second group the surgeon has to account for the tendency of Glucocorticoids (corticosteroids) to cause separation of healed or sutured incisions, increased risk of infection, and delayed healing of open wounds while continuing the glucocorticoid medication they need after surgery. Glucocorticoids produce these effects by interfering with inflammation, fibroblast proliferation, collagen synthesis and degradation, deposition of connective tissue ground substances, angiogenesis, wound contraction, and re-epithelialization. Vitamin A restores the inflammatory response and promotes epithelialization and the synthesis of collagen and ground substances. However, vitamin A does not reverse the detrimental effects of glucocorticoids on wound contraction and infection. The RDA for vitamin A is 3,000 IU per day. To reverse the effect of glucocorticoids on healing 10,000 IU per day for 2 to 3 weeks after surgery should suffice for those that are not vitamin A deficient and is well within the range of what could be toxic. This would have to be given in addition to the hydrocortisone, prednisone, dexamethasone or glucocorticoid that was being taken prior to surgery.
In summary before surgery your surgeon needs to know which specific glucocorticoid medication was prescribed/taken, what the doseage was, how long it was taken for, if was taken daily or intermittently and when it was stopped. All of these variables can impact the safety of your cosmetic surgery.





Join the Discussion!