Most of us know when we see a good result from breast surgery whether it be implants for breast augmentation or reconstruction after breast cancer surgery (mastectomy) or the results of a breast reduction surgery. As I described in my blog on facial proportions analysis a similar proportions assessment is used in planning any breast surgery and in assessing the end result.
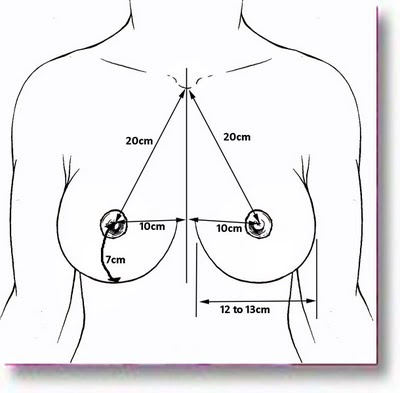
That is to say for the average woman between 5 and 6 feet tall the desired proportions are that the nipples form an equilateral triangle with the upper notch of the breast bone and each side of the triangle is about 20cm in length. Additionally the distance between each nipple and the fold under the breast should be about 7cm with a gentle curve outline along the bottom of each breast. Together with equal sized nipple areola complexes this creates the left right symmetry and aesthetic look we strive for. The question then arises as to how one achieves this goal or result after breast surgery. This blog will only deal with breast implants rather than breast reductions and mostly with options available to correct for deviations from this pattern after breast implant placement i.e. redo breast implant surgery when the nipple is in the correct position.
In planning/performing breast implant surgery the surgeon must diagnosis deviations from these proportions before surgery. In the non-reconstructive patients i.e. implants placed for breast augmentation the surgeon firsts addresses nipple position on each breast with respect to the breast bone notch and the fold under the breast. After that the breast tissue has to be centered under the original or corrected nipple position. Surgical adjustments of nipple position are in reality various degrees of breast lifting or mastopexy. The more lifting that is required the more skin has to be removed and the bigger/longer the skin scar. Then the breast implant has to be centered under all of that preferably with breast tissue overlapping the edges of the implant. If the implant goes past the edge of the breast tissue it may be visible as a second edge and we call that a double bubble. The double bubble can also appear when breast implants are placed under the chest muscle separate from the native breast tissue. As the patient ages the breast tissue can sag downward separating from the submuscular implant that is held in place by the chest muscle and thereby creating a double bubble deformity.
The average 12 to 13 cm breast base diameter patient gets an 11 to 12 cm diameter implant. If the implant is too large for the space under the breast the normally curved breast contour may be squared off or the 2 implants may touch across the midline. I had a short asian patient with an 11cm base diameter breast in whom another surgeon put a 13cm diameter implant and she ended up with squared breasts. After a simple change to a smaller base diameter the problem was resolved. That change did not alter the front to back projection of the breast because today we have a vast selection of implant sizes available.
Deviations from the above desired proportions can be due to surgeon, patient or implant related factors or any combination of these factors. The surgeon can pick the wrong implant or surgical technique. The patient may not follow instructions after surgery such as too early a return to exercise. Too large an implant overtime can shift in position. The patient’s body can react adversely to the implant by forming scar tissue around it that contracts thereby squaring off the contour. You can see there are lots of things that can become a problem during, shortly after or sometime after surgery.
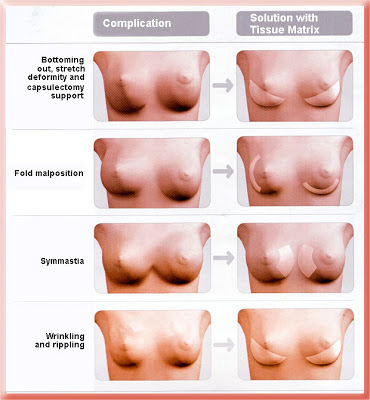 These problems can be classified as bottoming out, bad positioning of the fold under one breast, symmastia or synmastia and wrinkling or rippling as depicted on the left above. A combination can also occur such as bottoming out and rippling. Possible surgical solutions involving the placement of allogenic acellular dermal graft or tissue matrix are depicted on the right. This graft material is processed from human organ donors’ skin and all skin cells are removed to prevent rejection. The deep layers of skin that do not contain skin cells are left intact so what is left is basically a sheet of collagen. It has been used for a variety of purposes since the early 1990s, including skin grafting of burn wounds, nasal reconstruction, eyelid reconstruction, gum surgery etc. In the mid- 1990s plastic surgeons began using it for cosmetic surgery such as making the lips fuller. Use of the material in breast surgery followed.
These problems can be classified as bottoming out, bad positioning of the fold under one breast, symmastia or synmastia and wrinkling or rippling as depicted on the left above. A combination can also occur such as bottoming out and rippling. Possible surgical solutions involving the placement of allogenic acellular dermal graft or tissue matrix are depicted on the right. This graft material is processed from human organ donors’ skin and all skin cells are removed to prevent rejection. The deep layers of skin that do not contain skin cells are left intact so what is left is basically a sheet of collagen. It has been used for a variety of purposes since the early 1990s, including skin grafting of burn wounds, nasal reconstruction, eyelid reconstruction, gum surgery etc. In the mid- 1990s plastic surgeons began using it for cosmetic surgery such as making the lips fuller. Use of the material in breast surgery followed.
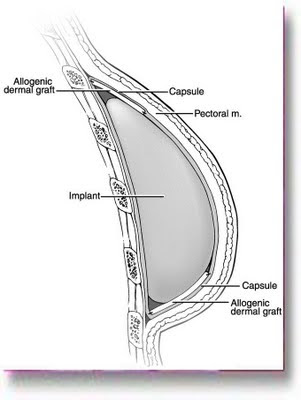
This is a cut away view of the breast showing how the graft can be sutured along the upper and/or lower edge of the implant as needed.
Bottoming out occurs when the implants shift position downward and are no longer (if ever) centered under the nipples. This can be due to disruption of the folds under the breasts, excessive disruption of chest muscle fibers near the midline breast bone at the time of surgery or development of a capsule that is so thin that it cannot withstand the pull of gravity on the implants. Surgical correction involves placing sutures between the under surface of the skin and the rib cage, suturing the capsule to itself under the implant or placing an acellular dermal graft at the bottom of the breast. The graft is sutured in place to reshape the fold.
The phenomena of bottoming out can be used in a controlled fashion to improve a result over time. For example in breast reduction surgery the nipple to fold distance is made slightly shorter because settling of the tissue over time with some bottoming out is expected and the surgeon is looking for a better long term result at the expense of a poorer short term result.
Synmastia or symmastia after breast augmentation – breast implant placement is a condition where the breasts meet across the chest midline with migration of one or both implants so they touch across the midline. Patients who have had multiple breast operations especially if done only to place sequentially larger implants, excessively large breast implants with large base diameters, or overaggressive surgical dissection across the midline are susceptible to developing synmastia. This is much less common than outward or downward shifting of the implants. It can also happen if too large an implant is placed so that the inner sides of the implants touch. In subtle cases you can only see the synmastia when you push on the implants but not when the patient just stands upright. This can occur with the implants above or below the muscle but appears to be more common when they are below the muscle. The treatment is suturing the capsule near the midline to itself and or placement of acellular dermal grafts at the inner edges of the breasts. If the patient has very large implants above the muscle this can also be treated by replacing them with smaller implants under the muscle.
Wrinkling or rippling is an inherent property of implants. Implants may look very good when lying flat on a table. However, when upright the upper portion of the implant collapses (wrinkles or ripples) as the implant contents fall to the bottom of the implant and can’t support the upper part of the implant.
If the implant is placed on top of the muscle in a thin individual with small breasts the collapsed upper part of the implant can be very unsightly when the patient stands upright. The collapsed edges appear as rippling when viewed from outside the body. The rippling becomes more apparent after the swelling from surgery resolves and the pocket around the implant shrinks to meet the dimensions of the implant. When placed under the muscle the rippling is more apparent to the side of the chest wall, where there is no muscle, and when leaning forward because this positions the implant closer to the surface. This rippling affect is more apparent and the implant edges are more visible with saline filled implants because of the chemical properties of salt water especially when the soft tissue (breast gland and fat) between the outside world and the implant is thinner. Rippling is least apparent with the cohesive gel implants because when upright or even with the implant shell removed the gel inside retains its shape.
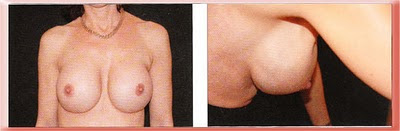 This patient had saline implants that were too large for her chest placed under the muscle. On standing upright these oversized implants give the breasts a vertical rectangular look instead of a smooth curved contour and when leaning forward the rippling of the implant is visible outside the area of muscle coverage.
This patient had saline implants that were too large for her chest placed under the muscle. On standing upright these oversized implants give the breasts a vertical rectangular look instead of a smooth curved contour and when leaning forward the rippling of the implant is visible outside the area of muscle coverage.
The treatment for rippling historically was to replace a saline implant with a gel implant and/or move an implant under the gland to a position under the muscle. Now there are more options available to treat this problem. The implants can be changed to cohesive gel, their position can be changed to under the muscle and/or acellular dermal matrix can be sutured above the portion of the implant that ripples in order to hide the rippling.
Comparison of Saline, Silicone Gel and Cohesive Silicone Gel
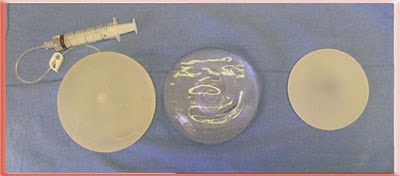 Top view lying flat Saline, Silicone Gel and Cohesive Silicone Gel
Top view lying flat Saline, Silicone Gel and Cohesive Silicone Gel
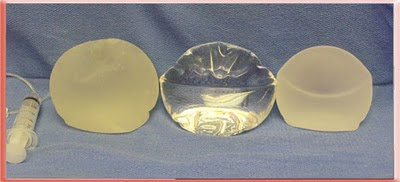 Front view standing upright Saline, Silicone Gel and Cohesive Silicone Gel
Front view standing upright Saline, Silicone Gel and Cohesive Silicone Gel
 Top view standing upright Saline, Silicone Gel and Cohesive Silicone Gel
Top view standing upright Saline, Silicone Gel and Cohesive Silicone Gel
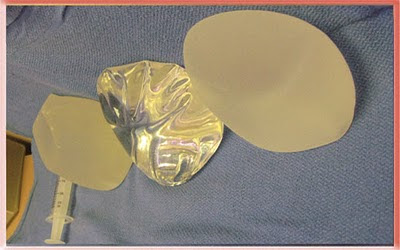 Oblique upper view standing upright Saline, Silicone Gel and Cohesive Silicone Gel
Oblique upper view standing upright Saline, Silicone Gel and Cohesive Silicone Gel
 Regular silicone gel and cohesive gel side by side
Regular silicone gel and cohesive gel side by side
These photos show the inherent properties of the implants. All three look the same when lying flat and viewed from above. They are quite different when upright as when a patient with breast implants stands up. The saline has the most rippling and the cohesive gel has the least.
Example Cases
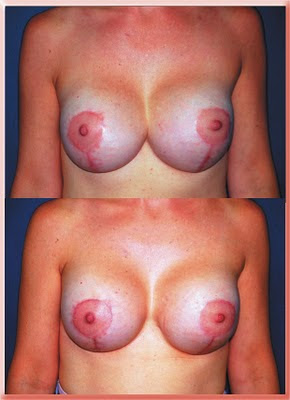 Symmastia following saline implant augmentation under the muscle and mastopexy breast lift and correction by placing acellular dermal grafts at the inner edge of each breast
Symmastia following saline implant augmentation under the muscle and mastopexy breast lift and correction by placing acellular dermal grafts at the inner edge of each breast
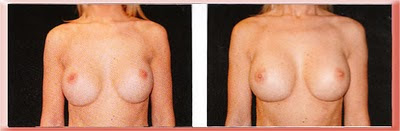
This case shows bottoming out of implants placed above the muscle. Moving the implants under the muscle corrected the problem by allowing the now overlying muscle to hold the implants in position so they do not drop with gravity. The after photo is 1 year after the corrective surgery.
The bottom line is there are currently more options available to treat these problems than there were in the past. Which option is best for a given patient is dependent on the patient and the experience of their surgeon. The main drawback to the use of acellular dermal grafts is that 1 sheet is required per breast and each sheet costs between $1000 and $2000. Currently most revisions using this material are for breast reconstructions after breast cancer surgery and so are covered by insurance. That is because revisions after cosmetic breast augmentation are not covered by insurance and the average patient cannot afford to pay up to $4000 just for the material used in surgery.
Aaron Stone MD – Plastic Surgeon Los Angeles
Aaron Stone MD – twitter


![]()

![]()





Join the Discussion!