Breastfeeding is a vital function for infant mother bonding, transmission of antibodies to the baby to fight infection etc. All women with breast implants and no other prior breast surgery giving birth at an Argentinian hospital between April 2013 and July 2014 were followed and compared to body matched mothers and babies. After giving birth those with breast implants had insignificantly lower success at breastfeeding at 30 days after giving birth than those women who did not have breast implants: 93% with implants vs. 97% without implants. Also, it did not matter whether the implants were placed via incisions in the crease under the breast or in the outer edge of the areola (skin around the nipple). Therefore we can conclude that most women can establish breastfeeding even if they have breast implants irrespective of how the implants were placed.
Breast Reconstruction with Aeroform Tissue Expander
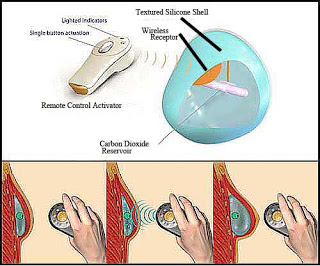
It seems like all the latest breast reconstruction techniques like Neopec come from Australia. Now the Australians have come up with a rapid way to expand chest skin after breast cancer mastectomy to allow placement of a breast implant and thereby reconstruct the breast (see my blog Reconstruction After Breast Cancer Surgery). Usually a saline balloon or expander is surgically placed and the surgeon then progressively fills it with salt water that is injected on a weekly basis to stretch the skin. This can take up to 6 months. Now they have devised an expander that contains a cylinder of compressed carbon dioxide gas. The patient controls the release of the gas into the expander with a handheld remote control and slowly expands on a daily basis.
Preliminary data reveal that using the Aeroform Tissue Expander the expansion can be completed in 17 days instead of 6 months. Enrollment in FDA clinical trials have begun in the US and the manufacturer is predicting a 2014 FDA clearance for general use.
Aaron Stone MD – Plastic Surgeon Los Angeles
Dr. Stone’s Twitter


![]()



New Type of Breast Implant – The Ideal Breast Implant
The 2 main types of breast implants available for decades have been the saline filled an silicone gel filled breast implants. Each has its pros and cons. Silicone gel implants have a more natural feel and look. Unlike silicone gel, implants containing only saline do not blend well with surrounding tissues at the edges of the implants. This is due to the chemical properties of salt water which is chemically charged as positive and negative charges that attract each other as opposed to silicone gel which does not carry a charge. Thus saline is more cohesive than silicone. What this means in clinical terms is that saline implant margins are more visible than silicone gel implant margins, especially when the soft tissue (breast gland and fat) between the outside world and the implant is thinner. Thus, in those patients with smaller breasts (less glandular tissue and/or fat) it is preferable to place saline implants under the chest muscle.
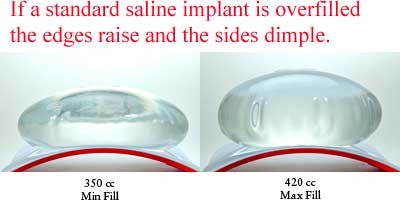
Saline implants may look very good when lying flat on a table. However, when upright the upper portion of the implant collapses (wrinkles or ripples) as the cohesive saline falls to the bottom of the implant and cannot support the upper part of the underinflated implant. If this underinflated implant is placed on top of the muscle in a thin individual with small breasts the collapsed upper part of the implant can be very unsightly. The collapsed edges appear as rippling when viewed from outside the body. The rippling becomes more apparent after the postoperative swelling resolves and the pocket around the implant shrinks to meet the dimensions of the implant. When placed submuscularly the rippling is more apparent to the side of the chest wall and lower chest, where there is no muscle, and when leaning forward because this positions the implant closer to the surface. Overfilling a saline implant (above the amount listed on the box) on the other hand can also be unsightly & doesn’t necessarily prevent the appearance of wrippling. Overfilling produces a hard breast which most patients seem to like less than rippling. Despite this some patients prefer saline because they are worried about leakage of silicone gel. Since the saline implants are inflated after placement they can be inserted through a much smaller incision than silicone gel implants and can be fine tuned for size and breast symmetry as they do not come pre-filled.
For years double lumen implants of saline and silicone gel were available in attempt to have a breast implant that was the best of both worlds. The implants had an adjustable saline bag inside a silicone bag.
They were available in 50/50, 25/75 and 35/65 percentage ratios of silicone gel to saline. I have recently been informed by the manufacturers that they no longer make this type of implant.
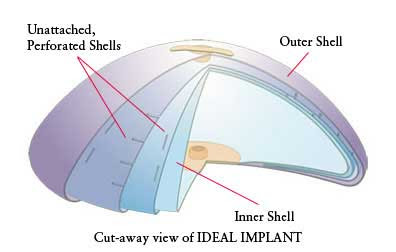
In 2006 a new saline implant was designed to improve the results obtainable with saline implants. It is called the Ideal Implant and contains an inner shell defining an inner saline compartment and an outer shell defining an outer saline compartment; between these shells are one to three unattached, perforated shells.
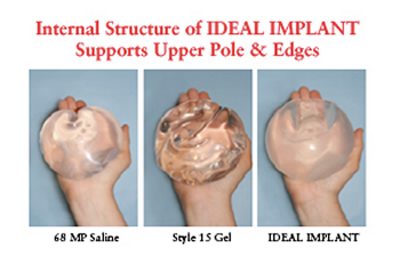
This internal structure was designed for control of saline movement to reduce bouncing, and for support of the implant edges to minimize wrinkling and prevent collapse of the upper portion of the implant. In the photo below you can see less collapse of the upper half of the Ideal Implant when it is upright.
The edges of the implant were also lowered so it may contour better to the chest wall.
FDA clinical trials were then begun and closed to new patients in 2010. The studies will last 10 years but the 2 year results have just been released and are favorable. Two-year follow-up visits were completed by 472 of the 502 women enrolled at 35 private practices. Of these, 378 had undergone primary breast augmentation and 94 had received replacement augmentation. Patient-reported satisfaction with the outcome was 94.3% for primary augmentations and 92.3% for replacement augmentations. Moreover, surgeon-reported satisfaction was also high (96.5% and 93.4%, respectively). The incidence of moderate-to-severe wrinkling was 3.8% (primary) and 12.0% (replacement). Baker Grade III and IV capsular contracture rates were 3.8% (primary) and 8.2% (replacement). These 2-year rates are lower than those reported for current standard single-lumen saline implants at 1 year. It will still be a number of years before these are available to the general public but it looks promising so far.
A Natural Look with Breast Implants
New Discovery Could Make Breast Implants Obsolete
Aaron Stone MD – Plastic Surgeon Los Angeles
Aaron Stone MD – twitter


![]()


Systemic Lupus Erythematosus (SLE) and Cosmetic Surgery
Lupus is a rheumatic condition which affects the muscles, joints, and connective tissue. About 1.5 million people in the US have lupus which includes as many as 10,000 children. Nearly 90% of those diagnosed with lupus are female. It’s an autoimmune disease. A healthy immune system produces special proteins or antibodies and these normally protect the body against bacteria and viruses that cause infections. In the case of lupus, the immune system confuses the body’s healthy cells and sees them
instead as if they were a bacteria or a virus, and the result is that our antibodies then attack some of our own body’s healthy cells. You become allergic to yourself.
So, what causes lupus? The cause is unknown although genetic factors may be important. Certain things can trigger the disease such as infection, medications, and even extreme physical or emotional stress. There are different types of lupus; the commonest is something called systemic lupus erythematosus or SLE and this affects multiple organs, and there is also form known as discoid or cutaneous lupus which only affects the skin, and in as many as 10% of all lupus cases, they’re classified as drug-induced lupus.
Systemic Lupus Erythematosus (SLE) is an autoimmune disease where self generated antibodies attack different organs systems in the body including blood vessels, liver, eyes, kidneys, joints, heart, heart valves, skin, lungs, brain…and/or form complexes with their protein targets (antigens) that damage these organ systems. The degree of damage to each organ system is highly variable. Arthritis and joint pain is the most frequent complaint. It is thought to be due to a genetic predisposition combined with viral infections. The disease can spontaneously remit, respond to corticosteroids or be unresponsive to available medications. 50% of those with SLE have some degree of heart and/or kidney involvement. Much of this organ damage can be masked and then suddenly become apparent especially during flare ups of the disease. I am aware of one women in her 30s who died in the recovery room after breast augmentation by another surgeon due to a heart attack caused by SLE induced damage to her coronary arteries.
So, what are the symptoms that are commonly associated with lupus? There are many. Classically, there will be butterfly rash. This is a rash that is across the cheeks and the bridge of the nose. There may be sensitivity to light that results in a rash. Also there can be ulcers in the nose or mouth, which are usually painless. There’s a long list of many other symptoms that are associated with lupus including things like arthritis, inflammation of the lining around the organ such as the heart and the
lungs, kidney problems. There may also be neurological disorders including problems with seizures or even psychosis. Blood problems and problems with the immune system are also found in lupus. And in addition to that, there are some nonspecific symptoms such as fever, weakness, fatigue, and weight loss. There is no known cure for lupus but the symptoms can be controlled with drugs, for example steroids, and sometimes more aggressive treatment is needed with immunosuppressive therapy.
Therefore it is imperative if you have systemic lupus that you have a complete examination of all major organ systems before undergoing any elective cosmetic surgery. This may include cardiac stress testing and blood tests for liver and kidney function. If you cannot be weaned off of prednisone that may be an ominous sign and may preclude any elective cosmetic surgery especially if any implants are involved.
If you are taking prednisone for lupus the medication can also prolong the healing time after surgery and weaken your ability to fight infection so proceed with caution before undergoing any elective cosmetic surgery.
For detailed information, support groups and to live the fullest life that you can with lupus visit the Lupus Foundation of America and the Lupus Research Institute.
Aaron Stone MD – Plastic Surgeon Los Angeles
Aaron Stone MD – twitter


![]()


Breast Implants and Bodybuilding
Female body builders in general have little body fat and the process can also melt away breast tissue. Refilling the breast skin envelope is then challenging in this situation because there is so too little fat or breast tissue to cover the edges of a breast implant placed on top of the muscle. So saline implants above the muscle are out of the question. Implants placed under the muscle are even more problematic because the pressures or forces applied to them during weight lifting can rupture the implant or more commonly shift them out of position. I saw one patient who while bench pressing squeezed her implant out of position so it formed an unsightly U-shape around the lower border of the pectoralis major chest muscle.
The only answer although not optimal is a cohesive gel breast implant placed on top of the chest muscle and in selective cases the addition of acellular dermal matrix to ensure the edges of the implant and rippling are not visible, although that is costly and is not the right choice for all such patients.
Breast Implants Augmentation and a Natural Look
Aaron Stone MD – Plastic Surgeon Los Angeles
Aaron Stone MD – twitter


![]()

![]()
Breast Implants and Lymphoma Cancer
Patients with either saline- or silicone gel–filled breast implants may have a very small but significant risk for a rare cancer called anaplastic large-cell lymphoma (ALCL), a cancer of the immune system, adjacent to the implant. This is currently under investigation and its existence should be considered if there is a build up or collection around the implant (seroma) years after the original surgery. Because the risk is very small the current policy is one of data collection only and no changes have been recommended for the use of breast implants or the frequency of follow up after breast implant surgery. The FDA continues to state that breast implants are “safe and effective when used as labeled.”
ALCL can occur anywhere in the body in the absence of breast implants. It is diagnosed in 1 of every 500,000 women per year in the United States. ALCL in the breast is rarer still, diagnosed annually in roughly 3 of every 100 million women without implants. In women with breast implants, it is usually inside the fibrous scar tissue — called a capsule — surrounding the implant. It is not a cancer of the breast per se.
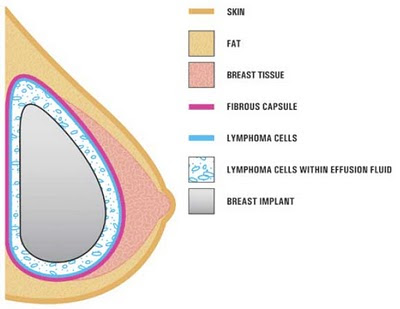 ALCL associated with breast implants is limited to the fluid inside the capsule and the inner wall of the capsule. It can occur whether the breast implants were placed for cosmetic (breast augmentation) or reconstructive purposes (reconstruction after breast cancer surgery).
ALCL associated with breast implants is limited to the fluid inside the capsule and the inner wall of the capsule. It can occur whether the breast implants were placed for cosmetic (breast augmentation) or reconstructive purposes (reconstruction after breast cancer surgery).
Treatment options for ALCL are chemotherapy, radiation, and surgery. The ALCL found related to breast implants is less aggressive and is sometimes treatable by simply removing the implant, the entire capsule, and the collected fluid resulting in a cure. Those patients who have had new implants placed at the time of lymphoma and prior implant removal have not had a recurrence of the lymphoma to date unless the previous capsule was not completely removed. The problem is in most capsulectomies with implant exchange the back wall of the capsule is frequently left at least partially intact. In cases with ALCL it is imperative that no capsule be left behind. An FDA review of scientific literature published from January 1997 through May 2010 uncovered 31 unique cases of ALCL in women with breast implants throughout the world. As of this writing the FDA is aware of 60 cases in all, some of them identified through other channels. The FDA does not know how many of the 60 may be duplicates of cases found in the literature. An estimated 5 million to 10 million women worldwide have received breast implants, according to the FDA.
Of the 31 published cases of ALCL, 24 involved silicone implants, and 7 saline implants. It is not known if the implant surface texture has any bearing on ALCL. The median time from implant to ALCL diagnosis was 8 years. For most of the women, the cancer was diagnosed when they sought treatment for implant-related pain, lumps, swelling, or asymmetry, after their surgical sites had healed. The main presenting symptom is an enlarged swollen breast 8 to 10 years after surgery in the absence of infection. Prophylactic breast implant removal in patients without symptoms or other abnormality is not recommended.
Because of the small number of cases worldwide the vast majority of plastic surgeons will not see a single case in a lifetime of practice and the current recommendations for women with breast implants are:
- Do not change your routine medical care and follow-up because ALCL is very rare; it has occurred in only a very small number of the millions of women who have breast implants Monitor your breast implants. If you notice any changes, contact your health care provider promptly to schedule an appointment.
- Get routine mammography screening.
- If you have silicone gel-filled breast implants, get periodic magnetic resonance imaging (MRI) to detect ruptures as recommended by your health care provider. The FDA-approved product labeling for silicone gel-filled breast implants states that the first MRI should occur three years after implant surgery and every two years thereafter.
The risk for breast cancer is 1 in 9 and the risk for ALCL is 1 in 500,000.
The American Society of Plastic Surgeons is collaborating with the FDA to develop a centralized registry to collect more information on existing case reports and any new cases that may be identified going forward. Only patients with confirmed ALCL will be entered into the registry. It is estimated that only 2 or 3 patients will be entered into the registry per year. It is imperative that late onset seromas are aspirated with a syringe and stained for specific proteins before proceeding. If the stains are positive additional imaging studies and oncologic consultation are required before proceeding with any surgery.
Aaron Stone MD – Plastic Surgeon Los Angeles
Aaron Stone MD – twitter


![]()

![]()
Breast Implants Augmentation Reconstruction and a Natural Look
Most of us know when we see a good result from breast surgery whether it be implants for breast augmentation or reconstruction after breast cancer surgery (mastectomy) or the results of a breast reduction surgery. As I described in my blog on facial proportions analysis a similar proportions assessment is used in planning any breast surgery and in assessing the end result.
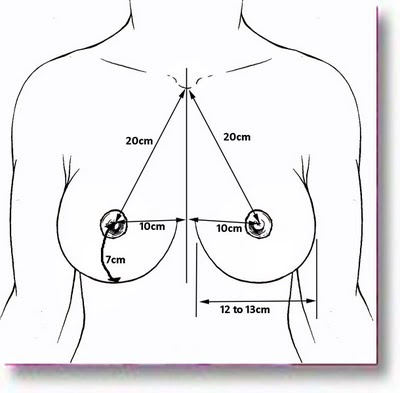
That is to say for the average woman between 5 and 6 feet tall the desired proportions are that the nipples form an equilateral triangle with the upper notch of the breast bone and each side of the triangle is about 20cm in length. Additionally the distance between each nipple and the fold under the breast should be about 7cm with a gentle curve outline along the bottom of each breast. Together with equal sized nipple areola complexes this creates the left right symmetry and aesthetic look we strive for. The question then arises as to how one achieves this goal or result after breast surgery. This blog will only deal with breast implants rather than breast reductions and mostly with options available to correct for deviations from this pattern after breast implant placement i.e. redo breast implant surgery when the nipple is in the correct position.
In planning/performing breast implant surgery the surgeon must diagnosis deviations from these proportions before surgery. In the non-reconstructive patients i.e. implants placed for breast augmentation the surgeon firsts addresses nipple position on each breast with respect to the breast bone notch and the fold under the breast. After that the breast tissue has to be centered under the original or corrected nipple position. Surgical adjustments of nipple position are in reality various degrees of breast lifting or mastopexy. The more lifting that is required the more skin has to be removed and the bigger/longer the skin scar. Then the breast implant has to be centered under all of that preferably with breast tissue overlapping the edges of the implant. If the implant goes past the edge of the breast tissue it may be visible as a second edge and we call that a double bubble. The double bubble can also appear when breast implants are placed under the chest muscle separate from the native breast tissue. As the patient ages the breast tissue can sag downward separating from the submuscular implant that is held in place by the chest muscle and thereby creating a double bubble deformity.
The average 12 to 13 cm breast base diameter patient gets an 11 to 12 cm diameter implant. If the implant is too large for the space under the breast the normally curved breast contour may be squared off or the 2 implants may touch across the midline. I had a short asian patient with an 11cm base diameter breast in whom another surgeon put a 13cm diameter implant and she ended up with squared breasts. After a simple change to a smaller base diameter the problem was resolved. That change did not alter the front to back projection of the breast because today we have a vast selection of implant sizes available.
Deviations from the above desired proportions can be due to surgeon, patient or implant related factors or any combination of these factors. The surgeon can pick the wrong implant or surgical technique. The patient may not follow instructions after surgery such as too early a return to exercise. Too large an implant overtime can shift in position. The patient’s body can react adversely to the implant by forming scar tissue around it that contracts thereby squaring off the contour. You can see there are lots of things that can become a problem during, shortly after or sometime after surgery.
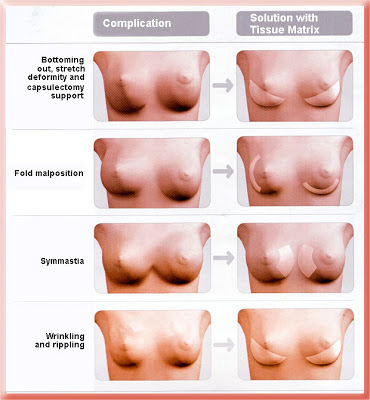 These problems can be classified as bottoming out, bad positioning of the fold under one breast, symmastia or synmastia and wrinkling or rippling as depicted on the left above. A combination can also occur such as bottoming out and rippling. Possible surgical solutions involving the placement of allogenic acellular dermal graft or tissue matrix are depicted on the right. This graft material is processed from human organ donors’ skin and all skin cells are removed to prevent rejection. The deep layers of skin that do not contain skin cells are left intact so what is left is basically a sheet of collagen. It has been used for a variety of purposes since the early 1990s, including skin grafting of burn wounds, nasal reconstruction, eyelid reconstruction, gum surgery etc. In the mid- 1990s plastic surgeons began using it for cosmetic surgery such as making the lips fuller. Use of the material in breast surgery followed.
These problems can be classified as bottoming out, bad positioning of the fold under one breast, symmastia or synmastia and wrinkling or rippling as depicted on the left above. A combination can also occur such as bottoming out and rippling. Possible surgical solutions involving the placement of allogenic acellular dermal graft or tissue matrix are depicted on the right. This graft material is processed from human organ donors’ skin and all skin cells are removed to prevent rejection. The deep layers of skin that do not contain skin cells are left intact so what is left is basically a sheet of collagen. It has been used for a variety of purposes since the early 1990s, including skin grafting of burn wounds, nasal reconstruction, eyelid reconstruction, gum surgery etc. In the mid- 1990s plastic surgeons began using it for cosmetic surgery such as making the lips fuller. Use of the material in breast surgery followed.
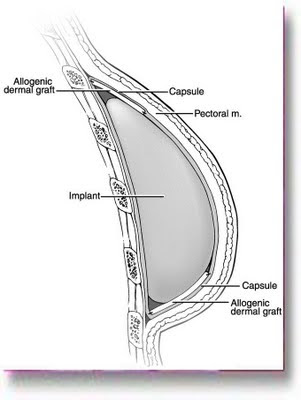
This is a cut away view of the breast showing how the graft can be sutured along the upper and/or lower edge of the implant as needed.
Bottoming out occurs when the implants shift position downward and are no longer (if ever) centered under the nipples. This can be due to disruption of the folds under the breasts, excessive disruption of chest muscle fibers near the midline breast bone at the time of surgery or development of a capsule that is so thin that it cannot withstand the pull of gravity on the implants. Surgical correction involves placing sutures between the under surface of the skin and the rib cage, suturing the capsule to itself under the implant or placing an acellular dermal graft at the bottom of the breast. The graft is sutured in place to reshape the fold.
The phenomena of bottoming out can be used in a controlled fashion to improve a result over time. For example in breast reduction surgery the nipple to fold distance is made slightly shorter because settling of the tissue over time with some bottoming out is expected and the surgeon is looking for a better long term result at the expense of a poorer short term result.
Synmastia or symmastia after breast augmentation – breast implant placement is a condition where the breasts meet across the chest midline with migration of one or both implants so they touch across the midline. Patients who have had multiple breast operations especially if done only to place sequentially larger implants, excessively large breast implants with large base diameters, or overaggressive surgical dissection across the midline are susceptible to developing synmastia. This is much less common than outward or downward shifting of the implants. It can also happen if too large an implant is placed so that the inner sides of the implants touch. In subtle cases you can only see the synmastia when you push on the implants but not when the patient just stands upright. This can occur with the implants above or below the muscle but appears to be more common when they are below the muscle. The treatment is suturing the capsule near the midline to itself and or placement of acellular dermal grafts at the inner edges of the breasts. If the patient has very large implants above the muscle this can also be treated by replacing them with smaller implants under the muscle.
Wrinkling or rippling is an inherent property of implants. Implants may look very good when lying flat on a table. However, when upright the upper portion of the implant collapses (wrinkles or ripples) as the implant contents fall to the bottom of the implant and can’t support the upper part of the implant.
If the implant is placed on top of the muscle in a thin individual with small breasts the collapsed upper part of the implant can be very unsightly when the patient stands upright. The collapsed edges appear as rippling when viewed from outside the body. The rippling becomes more apparent after the swelling from surgery resolves and the pocket around the implant shrinks to meet the dimensions of the implant. When placed under the muscle the rippling is more apparent to the side of the chest wall, where there is no muscle, and when leaning forward because this positions the implant closer to the surface. This rippling affect is more apparent and the implant edges are more visible with saline filled implants because of the chemical properties of salt water especially when the soft tissue (breast gland and fat) between the outside world and the implant is thinner. Rippling is least apparent with the cohesive gel implants because when upright or even with the implant shell removed the gel inside retains its shape.
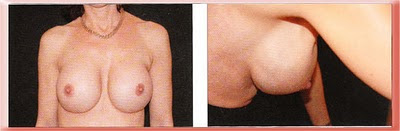 This patient had saline implants that were too large for her chest placed under the muscle. On standing upright these oversized implants give the breasts a vertical rectangular look instead of a smooth curved contour and when leaning forward the rippling of the implant is visible outside the area of muscle coverage.
This patient had saline implants that were too large for her chest placed under the muscle. On standing upright these oversized implants give the breasts a vertical rectangular look instead of a smooth curved contour and when leaning forward the rippling of the implant is visible outside the area of muscle coverage.
The treatment for rippling historically was to replace a saline implant with a gel implant and/or move an implant under the gland to a position under the muscle. Now there are more options available to treat this problem. The implants can be changed to cohesive gel, their position can be changed to under the muscle and/or acellular dermal matrix can be sutured above the portion of the implant that ripples in order to hide the rippling.
Comparison of Saline, Silicone Gel and Cohesive Silicone Gel
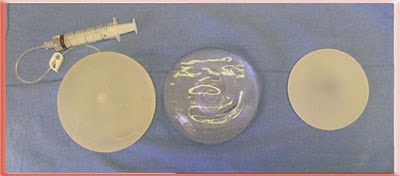 Top view lying flat Saline, Silicone Gel and Cohesive Silicone Gel
Top view lying flat Saline, Silicone Gel and Cohesive Silicone Gel
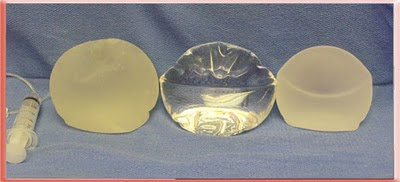 Front view standing upright Saline, Silicone Gel and Cohesive Silicone Gel
Front view standing upright Saline, Silicone Gel and Cohesive Silicone Gel
 Top view standing upright Saline, Silicone Gel and Cohesive Silicone Gel
Top view standing upright Saline, Silicone Gel and Cohesive Silicone Gel
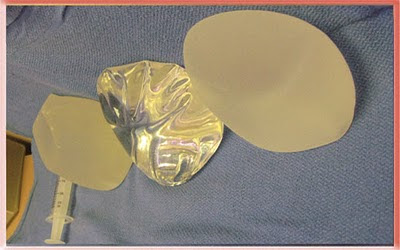 Oblique upper view standing upright Saline, Silicone Gel and Cohesive Silicone Gel
Oblique upper view standing upright Saline, Silicone Gel and Cohesive Silicone Gel
 Regular silicone gel and cohesive gel side by side
Regular silicone gel and cohesive gel side by side
These photos show the inherent properties of the implants. All three look the same when lying flat and viewed from above. They are quite different when upright as when a patient with breast implants stands up. The saline has the most rippling and the cohesive gel has the least.
Example Cases
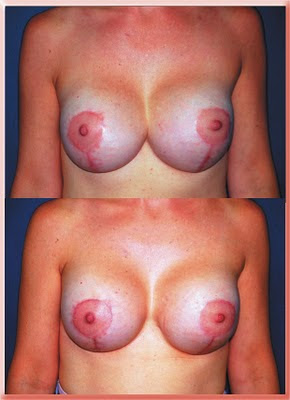 Symmastia following saline implant augmentation under the muscle and mastopexy breast lift and correction by placing acellular dermal grafts at the inner edge of each breast
Symmastia following saline implant augmentation under the muscle and mastopexy breast lift and correction by placing acellular dermal grafts at the inner edge of each breast
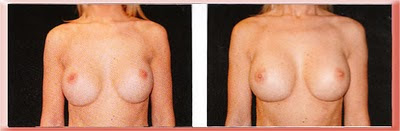
This case shows bottoming out of implants placed above the muscle. Moving the implants under the muscle corrected the problem by allowing the now overlying muscle to hold the implants in position so they do not drop with gravity. The after photo is 1 year after the corrective surgery.
The bottom line is there are currently more options available to treat these problems than there were in the past. Which option is best for a given patient is dependent on the patient and the experience of their surgeon. The main drawback to the use of acellular dermal grafts is that 1 sheet is required per breast and each sheet costs between $1000 and $2000. Currently most revisions using this material are for breast reconstructions after breast cancer surgery and so are covered by insurance. That is because revisions after cosmetic breast augmentation are not covered by insurance and the average patient cannot afford to pay up to $4000 just for the material used in surgery.
Aaron Stone MD – Plastic Surgeon Los Angeles
Aaron Stone MD – twitter


![]()

![]()
New Discovery Could Make Breast Implants Obsolete
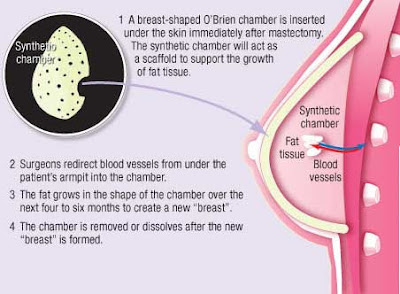
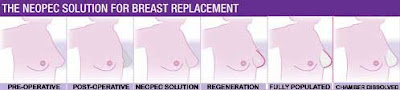
Earth shattering news out of Australia this week could have monumental effects on breast surgery, both reconstruction after breast cancer and enlargement for cosmetic reasons. The technique discovered in Australia is called Neopec. So far the process has only been performed in pigs and was so successful that human trials are scheduled too begin in early 2010. The pigs grew new breasts in 6 weeks. The surgeon places a scaffold or shell of biodegradable material in the breast, redirects a small blood vessel from the arm into the shell, places a small amount of the patient’s own fat inside the shell, and a dissolvable gel called Myogel is also placed in the shell. The Myogel and blood flow from the transferred artery stimulate the fat to grow until it fills the shell and therefore takes the shape of the shell. This is a direct finding from stem cell research. After that the biodegradable shell is dissolved by the body. In the future the shell may come with its own artificial blood vessel.
If this all works out breast implants for cosmetic breast augmentation or breast reconstruction would become obsolete. Also this procedure is much less taxing on the patient than a transfer of fat with intact blood supply to the breast from the lower abdomen or other areas of the body. It could readily available for breast reconstruction within 3 years and for cosmetic breast augmentation within 10 years.
The first few frames show the shells lying on the belly of a pig and the blue lines outline the blood vessels that will be redirected into the shells.
UPDATE MARCH 2011
The procedure will be called Neopec. The breast is scanned in order to obtain the measurements for the shell. The shell or chamber will be available within 3 days. The chamber is made of biodegradeable biocompatible synthetic material. The chamber is placed under the skin and a piece of armpit fat with its feeding artery intact is placed into the chamber. The fat grows to fill the dimensions of the chamber and the chamber dissolves over 3 or 4 months.
It is a 2 hour surgery with a 2 day hospital stay. The donor site scar is much smaller than that for surgery using abdominal fat or back fat-muscle. The result is permanent as long as your weight is stable.
Aaron Stone MD – Plastic Surgeon Los Angeles
Dr. Stone’s Twitter


![]()

![]()